Intestinal candidiasis. Causes
It is generally accepted that the gastrointestinal tract is the main endogenous reservoir of Candida, from where the subsequent spread of infection throughout the body occurs. Candida albicans belongs to the opportunistic flora and is a component of the normal intestinal microflora. Determination of the presence of Candida albicans in 10x4 degrees in a bacteriological analysis of stool, according to official requirements, is not an indication for making a diagnosis of “intestinal candidiasis,” much less for antifungal therapy. In practice, the clinician has to deal with candidiasis, which is observed in the intestines up to 80% and it is better for Candida to be below the detection level in the analysis (0).
Risk factors for the development of candidiasis infection are varied, they are also caused by various diseases of organs and systems of the body, in which signs of impaired intestinal microflora develop, in particular diabetes mellitus, oncopathology, inflammatory bowel diseases (Crohn's disease and ulcerative colitis), irritable bowel syndrome, anemia , AIDS, decreased immune defense, stress. Therapy for underlying diseases can also contribute to the development of intestinal microbiocenosis disorders and excessive growth of candida - this is the use of cytostatics, immunosuppressants, radiation therapy, antibiotics, and surgical interventions in the treatment.
The physiological periods of a person’s life, neonatality, pregnancy, menopause, old age, and deteriorating environmental conditions that reduce a person’s anti-infective resistance are also important in the occurrence of overgrowth of Candida fungi, which leads to an imbalance between the normal flora and the body’s immune response. (Burova S.A., Kurbatova I.V., 2006). All the reasons that were described above, in which a violation of the microbiocenosis of the gastrointestinal tract develops, can lead to candidiasis. The most significant conditions should be highlighted: gastric surgery, disorders of the secretory and motor functions of the stomach and intestines, colonic diverticulosis, and cirrhosis of the liver.
Poor nutrition and, in particular, steroids contained in food and supplements and food intolerance seem to be important for the development of dysbiosis of the gastrointestinal tract.
Why does the disease occur?
In small quantities, yeast-like fungi of the genus Candida are present in the body of any person. However, when immunodeficiency occurs, their active growth begins, the body’s defenses fail, and a disease occurs.
Various reasons can lead to a decrease in immunity. However, the biggest culprit is inappropriate or inappropriate use of antibiotics. They destroy “good” microorganisms in the intestines, which guard human health. Without them, the defense weakens and the infection takes over.
There are also negative factors that can provoke the disease. They are divided into 2 large groups:
- External.
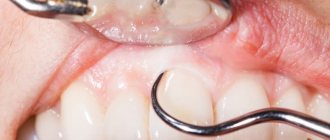
Thanks to them, the infection enters the body through damaged skin (burns, cuts, cracks). For example, damage to the oral mucosa can occur due to poor hygiene, periodontitis, and incorrectly selected dentures.
- Internal (endogenous).
These include diseases that lead to decreased immunity, as well as a congenital state of immunodeficiency. These are vitamin deficiency, hormonal imbalances, metabolic disorders, anemia, chronic gastrointestinal pathologies, diabetes mellitus.
Signs of candidiasis may appear due to frequent exposure of the skin or mucous membranes to chemicals. Taking hormonal contraceptives, alcohol abuse, smoking, unfavorable environment in the place of residence and frequent stress can also lead to the disease.
Intestinal candidiasis. Indications for examination
Indications for examination of the gastrointestinal tract to exclude fungal infection should be the following:
- the presence of 2 risk factors for the possible occurrence of candidiasis,
- double superficial colonization of candida,
- the presence of reasons that can lead to disruption of the microflora of the gastrointestinal tract with excessive growth of fungi of the genus Candida.
- febrile conditions of unknown origin, resistant to antibiotic therapy,
- skin and allergic diseases, because Candida is a trigger for allergic diseases and a factor favoring their development.
Algorithm for diagnosing intestinal microflora disorders with overgrowth of Candida flbicans:
- Analysis of medical history, identification of risk factors,
- analysis of clinical data,
- microbiological and gas chromatographic methods for studying disorders of the microflora of the intestinal tract (various biological environments),
- smears - impressions from the mucous membranes of the mouth and esophagus,
- if systemic candidiasis is suspected, it is necessary to culture blood and biological fluids and tissues for the presence of a fungal infection,
- serological diagnosis and assessment of the effectiveness of treatment based on the levels of antibodies to candida,
- inflammatory markers (lysozyme, a-antitrypsin, elastase),
- secretory immunoglobulin A, which allows assessing the degree of activity of the intestinal-associated immune system,
- immunological status (screening) level 1.
All laboratory data should be assessed and analyzed in conjunction with the patient's current clinical situation.
How is the disease diagnosed?
Visual methods for diagnosing candidiasis. Upon examination, inflammation of areas of the skin is revealed, limited to a border of exfoliating, macerated epidermis, and a whitish coating on the mucous membranes.
Laboratory diagnostics. Contrary to popular belief, the main method for diagnosing candidiasis is still microscopy of a smear from the affected areas of the mucosa. PCR (DNA diagnostics), which has become popular recently, is usually poorly suited for diagnosing candidiasis.
Laboratory diagnosis of the disease includes:
- microscopy of discharge smear
- cultural diagnostics (seeding)
- enzyme immunoassay (ELISA)
- polymerase chain reaction (PCR).
Intestinal candidiasis. Symptoms
Disturbances of intestinal microbiocenosis with excessive growth of fungi of the genus Candida or candidal dysbacteriosis are clinically manifested by fermentative dyspepsia, abdominal pain, more in the sigmoid region, flatulence, frequent abundant foamy loose stools with mucus are noted up to 6-10 times a day, accompanied by disturbances in vitamin metabolism, low-grade fever fever, severe weakness, headache. Symptoms of damage to the mucous membranes in the form of stomatitis, glossitis, and vulvovaginal thrush are often observed. Fungal infection sharply reduces immunity, which leads to a deeper development of visceral candidomycosis with damage to the upper respiratory tract, lungs, genitourinary and digestive systems. In the blood - moderate leukocytosis, accelerated ESR, with sigmoidoscopy - catarrhal hemorrhagic proctosigmoiditis.
Indications for therapy are subject to clinical, microbiological, serological or histological confirmation of candidal infection, detection of candida with clinical manifestations from two or more surfaces of fungal colonization.
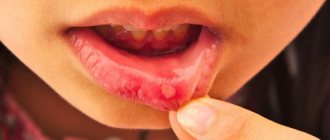
What does thrush look like in the mouth - its symptoms in adults
After Candida attaches to the mucous membrane, they multiply and “grow” deep into it2, causing inflammation, swelling and redness. There is a feeling of a “scalded mouth” and discomfort when eating and swallowing. There may be a change in taste and the appearance of a metallic, sour, salty or bitter taste1.
The proliferation of the fungus leads to the appearance of small white spots on the gums, tongue, inner surface of the cheeks and palate, reminiscent of curdled milk or grains of semolina porridge. Increasing in size, the “grains” turn into plaques, which, in turn, merge to form solid white films.
If plaques and films are removed with a spatula or a cotton swab (this does not require additional effort), then a bright red inflamed, eroded mucous membrane is revealed underneath them.
Oral mycosis can spread to the red border of the lips , causing redness, dryness and peeling. Seizures appear in the corners of the mouth: the skin becomes inflamed, covered with grayish-white scales and cracks5.
If candidiasis is not treated at this stage, the fungi “spread” to the tongue and pharyngeal tonsils.
When the tongue is damaged, glossitis develops - the tongue swells, its papillae are smoothed out, a characteristic white coating appears on its back and lateral surfaces1 - and when the pharyngeal tonsils are damaged, a sore throat occurs.
A sore throat caused by fungal microflora is very different from normal. With obvious inflammation of the tonsils and the presence of white films and plugs on them, there is no temperature or pain when swallowing, and the submandibular lymph nodes remain of normal size1.
Candidiasis can spread further - affecting the respiratory tract, causing pneumonia and blood poisoning, so it is important to stop the process at the very beginning.
Up to contents
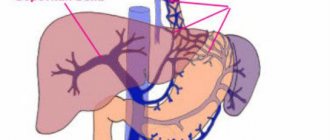
Localization of Candida
It should be noted that Candida primarily affects the stratified squamous epithelium of the oral cavity and esophagus and, less often, the single-layer cylindrical epithelium of the intestine. As a result, Candida fungi cause invasive lesions in the upper gastrointestinal tract and colonization (adhesion) in the areas below the stomach. At the same time, clinical symptoms discussed above as signs of non-invasive candidiasis may appear in the intestine, even at the adhesion stage. (Burova S.A., 2006). Consequently, among all localizations of candidiasis of the digestive tract, oropharyngeal candidiasis comes first, followed by candidal esophagitis, gastric candidiasis (often it can be suspected with ineffective Helicobacter pylori therapy and prolonged healing of the ulcer), intestinal candidiasis, which must be differentiated from pseudomembranous colitis caused by Clostridium difficile and acute process in the intestines caused by rotoviruses and Escherichia coli.
Risk factors for mucosal candidiasis
Defects in the antifungal resistance system briefly described above are factors contributing to the occurrence of candidiasis, or so-called. risk factors. Risk groups for the development of candidiasis of the digestive tract are presented below: • physiological immunodeficiencies (early childhood, old age, pregnancy); • genetically determined immunodeficiencies (for example, selective IgA deficiency); • iatrogenic immunodeficiencies – (for example, the consequences of treatment with glucocorticosteroids, immunosuppressants, anticytokine, radiation and polychemotherapy); • diseases of the endocrine system (for example, diabetes mellitus, autoimmune polyendocrine syndrome, hypothyroidism); • dysbiosis of mucous membranes after antibiotic therapy; • AIDS; • chronic “debilitating” diseases (for example, cirrhosis of the liver); • nutritional status disorders (for example, starvation and vitamin deficiencies).
In these groups, candidiasis is detected more often than usual. Note that sometimes the clear cause of the violation of antifungal resistance cannot be determined.
Intestinal candidiasis. Therapy
Therapeutic approaches to the treatment of gastrointestinal dysbiosis with overgrowth of Candida fungi include the following:
- A balanced diet excluding sugar and the consumption of complex carbohydrates, foods with prebiotic properties, and probiotic foods.
- Antifungal drugs.
2.1.Polyene antibiotics (nystatin, natamycin, levorin).
- Nystatin is most appropriate to use in the presence of candida in the esophagus, stomach and is practically ineffective when candida is localized in the intestine, which makes it also not effective when administered prophylactically along with antibiotic treatment.
- Pimafucin (natamycin) is the most effective drug for overgrowth of Candida in the intestines. The drug has an antifungal (fungicidal) effect. Interacts with sterols in fungal cell membranes, disrupting their structure and function and causing their death. Active against many pathogenic yeast fungi, especially Candida albicans. No resistance to natamycin was observed. For intestinal candidiasis, 1 tablet is prescribed. 4 times a day after meals for 7-10 days.
2.2. Triazole derivatives (flucanazole, Diflazon, Diflucan, Mikosist, Flucostat, rumicosis, intraconazole, terbizil, etc.), caspofungin derivatives - Cancidas (for administration of the drug), Noxafil (posaconazole) suspension for oral administration.
2.3. MPH (copper derivative of chlorophyll) is a plant antiseptic from brown algae, a natural immunomodulator due to stimulation of phagocytosis and the activity of copper cations, enhanced by the influence of alcohol, has a bactericidal effect against staphylococci, streptococci, pneumococci, fungi, putrefactive bacteria and E. coli and an antiviral effect. MPH protects and stimulates hematopoiesis, the anti-inflammatory effect is due to an excellent complex of microelements. Prescribed by a doctor orally, 1 drop per 5 kg of body weight daily in a small amount of water. The course of treatment is 30 days,
2.4. Citrosept is a herbal antimicrobial agent made from grapefruit seed extract, which has a bactericidal effect, including. and against fungi of the genus Candida and Helicobacteriosis of the stomach, promotes the absorption of vitamin C, contains bioflavonoids that strengthen the vascular wall of capillaries and prevent blood clots and cholesterol plaques, stimulates the body's natural resistance. It is prescribed as drops diluted in water or juice in different dosage regimens depending on the disease.
2.5. Self-eliminating bacillary preparations (B subtilis, L.bulgaricus) - Flonivin-IS, Baktisubtil, Sporobacterin, biosporin, Baktisporin, Gastrofarm, etc.
2.6. Saccharomyces boulardi - Enterol, 1 capsule contains 250 mg Saccharomyces boulardi, suppresses the growth of opportunistic flora and fungi Candida Krusei, Candida pseudotropical
2.7. Probiotics – lactose-containing preparations (Lactobacterin, Gastrofarm, Primadophyllus, Acidophyllus, Narine, etc.)
- Enterosorbents.
- Hepatoprotectors (Heptral, Hofitol, Karsil, milk thistle preparations, Floravit, etc.)
- Immunomodulatory drugs (Kipferon, Polyoxidonium, Dopolan, Marispan, etc.)
CANDIDIASIS OF THE ESOPHAGUS
Candidiasis is an infectious disease of the mucous membranes, skin and internal organs caused by yeast-like fungi of the genus Candida. Esophageal candidiasis (OC), which is a manifestation of visceral candidiasis, occupies a prominent place among infectious lesions of the esophagus. In recent years, there has been a tendency to increase the frequency of CP, especially in patients with impaired immunity. The growth of candidiasis infection is largely due to an increase in the number of patients with HIV infection, advances in transplantation and immunosuppressive therapy, and the uncontrolled use of antibiotics. KP occurs in 0.7-1.5% of gastroenterological patients [5, 6].
The problem with severe fungal infections caused by opportunistic pathogens is that they are difficult to treat and can be fatal. The mortality rate for invasive candidal infections has been found to be 34% [16].
Etiopathogenesis. Candida species are the most common esophageal pathogen, most notably Candida albicans, with occasional occurrences of C. tropicalis, C. parapsilosis, C. glabrata, C. lusitania, and C. krusei. These microorganisms are normal components of the oral flora and their growth is inhibited by bacterial commensals. Infection with fungi such as Candida, which are widespread in the environment, occurs through endogenous or exogenous routes. Endogenous infection is associated with the activation of saprophytic fungi; exogenous infection can occur through direct contact with carriers of infection or from the environment. If the host's body is not weakened, many fungi do not exhibit their pathogenic properties. Research in recent years has shown that the source of fungal dissemination is the intestines, and candidiasis of the oral cavity, genitals, and esophagus is a manifestation of systemic candidiasis. The likelihood of developing systemic damage depends both on the properties of the microorganism itself (their number, virulence, genetic and species heterogeneity of the population), and on the state of the macroorganism, especially its immune system, nutritional status and abdominal blood flow [3, 17].
Favorable conditions for the development of the infectious process are created by various violations of the physiological, anatomical and immunological mechanisms of the body's defense. Factors that provoke the occurrence of esophageal candidiasis include the use of antibiotics, inhaled or injected corticosteroids, antacid therapy or a hypochlorhydric state, diabetes mellitus, alcoholism, the consequences of intoxication, malnutrition, old age, impaired motility of the esophagus or esophageal obstruction, organ and bone marrow transplantation , enteral and especially parenteral nutrition, etc. A weakened immune system can lead to candidiasis infection. In diabetes mellitus, elevated blood glucose levels promote fungal growth because hyperglycemia impairs granulocyte function. Hypofunction of the parathyroid glands and adrenal glands leads to disruption of calcium-phosphorus metabolism, which causes hidden spasmophilia of the esophagus, thereby reducing its local protective capabilities [9]. Impaired nutritional status due to a lack of protein in the body and low calorie food affects the state of the immune system and creates the preconditions for the development of candidiasis [3]. Risk factors for candidiasis include a decrease in the acidity of gastric juice (pH 7.4 is optimal for the growth of Candida fungi, and when the pH shifts to 4.5, fungal growth is completely inhibited) [3, 4, 7].
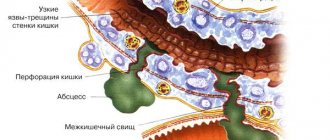
The pathological manifestations of KP are varied. At first, the affected areas of the esophagus have the appearance of individual whitish or yellowish lesions raised above the mucous membrane. Later, these lesions can merge, forming dense plaques with the introduction of the fungus into the submucosa or pseudomembranous deposits with the penetration of the fungus into the muscular layer and blood vessels [9]. Films that form on the esophageal mucosa in especially severe cases can almost completely close the lumen of the esophagus. Plaque consists of desquamated epithelial cells that mix with fungi, inflammatory cells and bacteria. Microscopic examination reveals uniformly colored yeast-like cells and filaments of mycelium of Candida fungi [9]. True ulceration is observed infrequently and in most cases is observed in immunosuppressed patients with granulocytopenia [29]. Sometimes necrosis of the esophageal wall occurs and phlegmonous inflammation of the esophagus and mediastinum develops, which can become one of the causes of death of the patient [1].
There is a morphological classification, according to which all cases of KP are divided into three groups depending on the severity of the process, that is, depending on the depth of damage to its wall: 1st group - individual whitish plaques with the introduction of pseudomycelium of the fungus between the epithelial cells; 2nd group - membranous plaques merging with each other and forming vast fields, while filaments of pseudomycelium grow not only the mucosa, but also the submucosa; Group 3 - pseudomembranous overlays, combined with deep changes, in which the threads of the fungus penetrate deeply into the thickness of the muscle tissue [10].
Clinical manifestations and complications. Symptoms of the disease are practically absent in 25-30% of patients suffering from KP, especially in immunocompetent individuals. However, most patients present with complaints related to damage to the gastrointestinal tract. The most typical clinical manifestations of KP are dysphagia and, somewhat less commonly, odynophagia. The severity of esophageal symptoms ranges from moderate difficulty swallowing to severe pain, resulting in the inability to eat and the development of secondary dehydration. In severe odynophagia, there may be other causes or co-infection, especially in patients with AIDS. Much less frequently, patients may complain of chest pain not associated with swallowing, heartburn, nausea, sometimes vomiting with the release of films (pseudomembranes), decreased appetite and weight, and the appearance of loose stools with mucus (see figure) [4, 9, 29].
| Symptoms of candidal esophagitis (RS Orlando, 1996) |
Physical examination may be helpful in KP. Approximately two thirds of patients with
AIDS and esophageal candidiasis have candidal stomatitis. KP is observed in patients with chronic mucocutaneous candidiasis, which is a severe form of candidal infection and is more often observed with dysfunction of the adrenal glands and parathyroid glands [29].
Complications of esophageal candidiasis are rare. Esophageal bleeding can be observed in severe cases of the disease, accompanied by the formation of erosions, ulcers, and be associated with coagulopathy; perforation may develop. Secondary obstruction of the lumen by mycetoma has been described. Necrosis rarely occurs with the development of phlegmonous inflammation of the esophagus and mediastinum [1]. In severe cases, specific esophagitis can be complicated by the development of candidiasis sepsis [6].
Diagnostics. Suspicion of esophageal candidiasis should arise in any patient if there are risk factors for the development of esophageal infection and complaints of dysphagia and odynophagia. The presence of candidal stomatitis confirms this diagnosis, but in its absence, damage to the esophagus is also not excluded.
Barium x-ray of the esophagus is usually used for initial evaluation before endoscopy. However, in the early stages of candidal esophagitis, X-ray examination of the esophagus does not have much diagnostic value, since it reflects only nonspecific changes common to all esophagitis [2]. Classic radiographic signs of acute esophagitis caused by Candida spp. are linear or irregular filling defects with clear edges. In severe cases of candidal esophagitis, fusion of lesions occurs, which is why large filling defects sometimes form clusters in the form of bunches of grapes [2]. In this case, the esophagus acquires a “shaggy” (“hairy”) appearance, simulating ulceration [25]. The presence of large, well-circumscribed ulcers is not a sign of candidal esophagitis. Impaired motility and narrowing of the lumen of the esophagus due to pseudomembranes may occur. It should be remembered that a normal barium radiograph of the esophagus does not exclude esophageal candidiasis. Due to severe odynophagia, the patient will not be able to drink barium, which makes X-rays of the esophagus difficult [29].
The double contrast radiological method is considered more informative for the diagnosis of candidal esophagitis, the effectiveness of which reaches 70% [26].
A cytology brush and balloon catheter are used to quickly diagnose esophageal infections without endoscopy. These instruments can be easily inserted through the nasal passages or the mouth through a protective probe that prevents contamination. The material obtained from the protected brush or balloon catheter after it is removed from the esophagus is evaluated cytologically and culturally. The technique using protected brushes has a sensitivity of 88% and a specificity of almost 100% [26].
The cytological method involves staining impression smears or swab sediment from a cytological brush in search of active forms of Candida - budding yeast cells, pseudomycelium and mycelium. The cultural method involves placing the test material on Sabouraud's glucose-enriched medium or other media, in order to then judge the etiology of the infectious process in the esophagus by the nature of the colonies formed.
Endoscopic examination of the esophagus is the most sensitive and specific method for diagnosing esophageal candidiasis. The endoscopic picture of KP is most often characterized by the presence of easily removable fibrinous loose overlays of white or yellow color, under which easily wounded and/or edematous mucosa is found. Catarrhal and erosive-ulcerative esophagitis are less common [19]. Candida spp. rarely causes true ulceration. The presence of an ulcer in candidal esophagitis is often a sign of an additional pathological process in the esophagus [29]. There are various endoscopic classifications of esophageal candidiasis (Tables 1 and 2).
During endoscopy, affected areas of the mucosa may be subjected to brush biopsy for cytological examination or biopsy for histological diagnosis. When ulcers are identified endoscopically, repeated biopsies help rule out the presence of coexisting pathological processes. Cytological examination of brush biopsy material has a higher sensitivity level than histological examination of biopsy specimens for mild superficial candidiasis because microorganisms may be washed off the tissue surface during processing of the biopsy material [19]. In rare cases, positive cytology in the presence of negative histology indicates colonization rather than infection. For more severe candidiasis of the esophagus, the greatest diagnostic value is histological examination of mucosal biopsies using special staining for neutral mucopolysaccharides according to Schiff PAS (CHIK reaction) or according to Gomori with silver hexamethylenetetramine. Only histological examination demonstrates invasion of the mycelium or pseudomycelium of the fungus deep into the tissue of the esophagus.
Skin testing and serological tests are not very informative for diagnosing esophageal candidiasis.
Treatment. There are many oral and intravenous medications that are used to treat candidiasis esophagitis. Despite the relatively wide choice of drugs, the treatment of KP is an urgent problem, since some drugs are not effective enough, others have serious side effects; In addition, there is currently an increase in resistance to antifungal drugs.
When treating KP, oral therapy should initially be prescribed; intravenous administration is used only in case of refractory disease or if there are contraindications to oral use of medications. Patients with moderate severity of the disease and minimal immunocompromise require a short course of therapy using systemically absorbed drugs such as oral azole. Immunocompromised transplant patients and AIDS patients with KP are best treated with longer courses of azole. In patients with granulocytopenia, when there is a significant risk of dissemination of Candida infection, the use of intravenous systemic drugs (azoles, amphotericin B) is justified [29].
The arsenal of modern antifungal agents is quite wide. Antifungal drugs of several groups are used to treat esophageal candidiasis. The most effective drugs are from the azole group. Non-absorbable azoles (clotrimazole, miconazole) are used orally; however, systemic drugs from this group (ketoconazole, fluconazole and itraconazole) are more effective. These drugs, like others in the azole group, alter fungal cell membrane permeability through cytochrome P450 (CYP)-dependent interference with ergosterol biosynthesis, resulting in fungal cell damage and death. New triazoles (itraconazole and fluconazole) have higher affinity similarity than imidazoles (miconazole and ketoconazole) for fungal CYP enzymes [14]. Although other drugs, such as miconazole, clotrimazole, and nystatin, can be used to treat candidal stomatitis, as well as to prevent esophageal lesions, these drugs are less effective as the main group of drugs for the treatment of KP [24].
Clotrimazole and miconazole are imidazole drugs. Clotrimazole tablets and miconazole for oral use are currently available. However, they are not absorbed from the gastrointestinal tract. These drugs can be used for mild candidiasis of the esophagus in people without immunodeficiency.
Ketoconazole (nizoral, oronazole) is an imidazole derivative and, when taken daily in a dose of 200 to 400 mg, gives a good effect in the treatment of esophageal candidiasis. In AIDS patients who usually require higher doses of ketoconazole, the daily dose can be increased, if nausea does not occur, to the maximum (800 mg). Ketoconazole penetrates well into various organs and tissues, but poorly through the blood-brain barrier. The drug is well absorbed from the gastrointestinal tract, but requires an acidic environment for optimal absorption. With gastric hypochlorhydria and the use of antacids, its bioavailability decreases. To improve absorption, ketoconazole should be taken 2 hours before taking antiulcer medications. Approximately 10-25% of AIDS patients experience decreased gastric acid secretion. Ketoconazole can cause a temporary blockade of the synthesis of testosterone and cortisol [6, 8, 29].
Itraconazole (Sporanox) belongs to the group of triazoles, like ketoconazole, and is prescribed at a dose of 200 mg per day. Further increases in the dose lengthen the half-life of the drug and increase its effectiveness. The absorption of intraconazole decreases when the pH of gastric juice decreases [23]. Ketoconazole and itraconazole are metabolized in the liver and excreted in the bile. The half-lives of these two drugs are 7 to 10 hours and 24 to 42 hours, respectively [14]. No dose adjustment is required in patients with renal failure.
Fluconazole (Diflucan, Diflazon, Forkan, Flucostat - domestic fluconazole) is a water-soluble triazole and is prescribed at a dose of 100 mg per day. Fluconazole is a drug whose absorption is independent of gastric pH and is significantly more effective in the treatment of esophageal candidiasis in AIDS than ketoconazole (200 mg daily) [21]. Fluconazole is available for oral and intravenous use. It is minimally metabolized and excreted unchanged in the urine. Fluconazole has a high tissue tropism and does not affect the synthesis of androgens and penetrates well through the blood-brain barrier. Unlike ketoconazole and intraconazole, it is highly soluble in water and minimally protein bound. The drug has a long half-life (approximately 30 hours, unless renal function is impaired and the presence of food or hypochlorhydria does not alter absorption), allowing it to be taken once daily. It has been shown that the administration of fluconazole improves immune parameters in the T- and B-systems [18]. Both fluconazole and itraconazole can be taken orally as solutions. These forms may be more effective than tablets because they enhance the local effect and improve absorption.
Adverse effects of ketoconazole, fluconazole and itraconazole are primarily dose dependent and include nausea, hepatotoxicity, decreased steroid production and cyclosporine metabolism [14]. In rare cases, ketoconazole can cause fatal hepatitis [12]. A slight increase in aminotransferases is a common side effect of all three drugs, but this should not be used as an excuse to discontinue them. The effect on steroidogenesis is most pronounced with ketoconazole. Reversible inhibition of gonadal and adrenal steroid synthesis by ketoconazole may occur when the dose exceeds 400 mg per day [27]. At recommended doses, fluconazole and itraconazole do not affect steroidogenesis. As a result of their effects on hepatic microsomal enzymes, all three azoles inhibit the metabolism of cyclosporine, which leads to an increase in the level of cyclosporine in the blood; this effect is most pronounced with ketoconazole [14].
Another main group of antifungal agents is polyene antibiotics, represented by amphotericin and nystatin. These drugs irreversibly bind to sterols in fungal cell membranes, thereby altering the permeability properties of the membrane, disrupting its barrier function and causing cell death. Nystatin (anticandin, mycostatin, fungicidin) is practically not absorbed from the gastrointestinal tract. It is used to treat candidal stomatitis, but is less effective in cases of esophageal candidiasis. In addition, the effectiveness, safety and ease of use of azole derivatives make it possible to consider nystatin as a second-line therapy. Amphotericin B (amphostat, fungizone) is the only polyene antibiotic for parenteral administration. It is not absorbed in the gastrointestinal tract, is used intravenously, penetrates well into various organs and tissues, and is excreted from the body by the kidneys. The half-life is 24-48 hours, but with systematic use it can increase to 15 days due to accumulation in tissues [8]. Although amphotericin B is the most effective drug used to treat systemic mycoses, its use in the treatment of KP is limited due to serious side effects. Side effects of amphotericin include neurotoxicity, hematoxicity, nephrotoxicity, local irritation (phlebitis), allergic reactions, dyspeptic disorders, fever, etc. [8]. The most adverse side effect resulting from long-term use of amphotericin is nephrotoxicity, which is usually reversible. This medication is now available as an oral solution and lozenges. In patients with KP who are refractory to treatment with fluconazole or other azoles, low doses of intravenous amphotericin B (10 to 20 mg daily) may be effective. The total dose of the drug for the treatment of esophageal candidiasis ranges from 100 to 200 mg [29].
Flucytosine is a drug with a narrow spectrum of antifungal activity that works by interfering with RNA translation. It is incorporated into fungal cells, where it is converted into 5-fluorouracil and inhibits thymidylate synthetase. This oral drug, which is given at a dose of 50 to 150 mg/kg per day every 6 hours, can be used in combination with amphotericin B, but it should not be used as monotherapy because fungi quickly become resistant to it. In addition, flucytosine monotherapy appears to be only moderately effective [12].
The newest class of antifungal drugs are candins, which interfere with the synthesis of the fungal wall. They are effective against most Candida species, including C. krusei. The first studies showed that capsofungin, which represents this group of drugs, was as effective in KP as amphotericin B [16].
When treating patients with KP, one should take into account the presence of resistance, which has now increased significantly due to the widespread use of azoles. If resistance develops, it is often useful to increase the azole dose. If this is not enough, switch to another drug from this group or use an oral solution of itraconazole [13], which must be prescribed in higher doses due to frequently observed cross-resistance. When a high dose (i.e. 400 mg daily) of fluconazole is not enough, switch to intravenous amphotericin B, and the result is achieved in 90% of cases. Resistance to amphotericin is rare [29].
In table 3 presents the treatment of candidal esophagitis depending on the function of lymphocytes and granulocytes.
In the treatment of candidal esophagitis in patients with AIDS, the first-line drugs are ketoconazole and fluconazole, with fluconazole being preferred. Due to better tolerability, it is primarily indicated for patients at an advanced stage of the disease who have many comorbidities. If swallowing is impaired, parenteral forms of fluconazole can be used. If first-line drugs are ineffective, drugs from the reserve group (amphotericin B, itraconazole), which are more toxic and/or more expensive, are used. Etiotropic therapy of esophageal candidiasis, in addition to the main course of treatment, requires maintenance treatment, which can be lifelong (Table 4) [4].
Treatment of candidiasis against the background of severe immunodeficiency and leukopenia is a difficult task. Along with antifungal therapy, it is important to restore the pool of neutrophil leukocytes and their functional activity, since neutrophil leukocytes are one of the main links in the defense mechanism against Candida spp. It is proposed as an additional agent in the treatment of candidal infection against the background of neutropenia to use granulocyte colony-stimulating factor, which reduces the deficiency of myeloperoxidase in neutrophil leukocytes and enhances their oxygen-dependent anti-candidal activity [7]. A good effect has been obtained from the endoscopic administration of granulocyte concentrate and high-intensity pulsed laser radiation to patients with KP, which improves immune functions [5].
Thus, to achieve success in patients with severe fungal infections, including candidiasis, an integrated approach to diagnosis and treatment is advisable. Increased survival will be facilitated by prompt diagnosis followed by the selection of effective specific antifungal therapy and therapeutic measures aimed at increasing the number of granulocytes and stimulating phagocytosis [16].
For questions about literature, please contact the editor
Intestinal candidiasis. Prolonged treatment
The duration of treatment is at least 6 weeks, and then prolonged pulse therapy in short courses with individual selection of drugs for 6 months, but observing the principles of prolonged treatment of gastrointestinal dysbiosis with overgrowth of Candida fungi.
- Rational nutrition continues mainly with the limitation of sugar-containing foods and dishes.
- Repeated courses of citrosept.
- Lactose-containing probiotics 10 days each month.
- Immunomodulatory drugs (repeated courses after 3 months)
- Hepatoprotectors – 2 courses over 6 months.
Assessment of the treatment effect according to the clinical and laboratory data discussed above, during treatment and after 6 months.
Types of disease
The clinical picture of oral candidiasis is classified:
- For clinical and morphological.
- With the flow.
- By localization.
Clinical and morphological is divided into:
- Hyperplastic.
- Erosive-ulcerative.
- Pseudomembranous.
- Atrophic.
The clinical picture, classified according to the course, is divided into:
- Chronic.
- Spicy.
By localization:
- Cheilitis.
- Gingivitis.
- Glossitis.
- Stomatitis.
- Tonsillitis, etc.
Based on the clinical picture, oral candidiasis comes in several types:
- Chronic hyperplastic.
- Candida infection.
- Chronic atrophic.
- Acute pseudomembranous.
- Chronic pseudomembranous.
- Acute atrophic.
Symptoms
Infection of the oral mucosa by Candida fungus can take various forms, each of which has its own characteristics of symptoms. The most common forms of the disease are candidal angulitis, glossitis, cheilitis, and stomatitis. There are both acute and chronic forms of the disease.
- Pseudomembranous acute candidiasis is the most common form and most often occurs in infants and the elderly. This form is characterized by the appearance of severe swelling and hyperemia (redness) of the mucous membranes. In addition, a characteristic whitish coating forms on the surface of the lips, palate, back of the tongue and the inside of the cheeks. If the plaque is scraped off, the surface of the mucous membrane underneath will be macerated (softened) or ulcerated and bleeding. In this case, patients complain of pain, burning or itching in the mouth; Eating becomes very difficult. Very often the process spreads to the esophagus and pharynx.
- Acute atrophic candidiasis of the oral mucosa usually develops due to the lack of adequate treatment. The upper part of the mucous membranes (epithelium) is exfoliated, the mucous membrane becomes thin, red or, on the contrary, swollen. The patient’s tongue and the corners of the lips also acquire a bright red color; the papillae on the tongue atrophy and smooth out. The plaque is absent or is found only in hard-to-reach places.
- Hyperplastic chronic candidiasis is characterized by the formation of a large number of papules and plaques of irregular or round shape. They are located close to each other on the mucous membrane of the tongue and cheeks and often become soldered and fused. Around each such formation there is a thin rim of reddened, inflamed tissue. It is difficult to scrape off or otherwise remove such a plaque. The oral cavity becomes dry and rough; When chewing, speaking, and even at rest, patients experience significant discomfort and pain. It should be noted that this disease most often affects men over 30 years of age.
The main cause of the chronic atrophic type is constant injury to the mucous membranes, for example due to wearing a prosthesis. Symptoms of the disease are localized in the affected area. Redness of the mucous membrane occurs (often along the contour of the lesion), plaque forms, pain and burning occur, and the membranes become dry.