Back
Hepatitis and cirrhosis of the liver are common diseases of various etiologies, which are manifested by jaundice and occur when hepatocytes are damaged and bile stagnation. This leads to serious disruptions to the functioning of the entire body, including death.
Author:
- Nikonov Mikhail Yurievich
(Voted by: )
Many of us begin to think about the state of our health only when we hear an alarm bell from it, or even several. This also applies to the liver, the hottest organ of our body, which bears special responsibility for numerous and very important processes occurring in it.
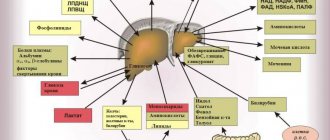
For example, our liver courageously takes on the first “blow” of toxic substances, allergens and other substances that are unsafe for us (including metabolic products), practically transforming them into safer ones and ready for elimination from the body. It also comes with an excess of hormones, vitamins and other elements that are beneficial to us in normal doses.
On the other hand, the liver accumulates reserves of useful substances (for example, glycogen, vitamins and microelements) to regulate carbohydrate metabolism and a large amount of blood (in case of emergency compensation for blood loss). The liver also synthesizes hormones and enzymes, blood plasma proteins, cholesterol and lipids, bile (including the specific pigment bilirubin), without which our body simply could not exist.
During our lives, the liver copes with such a huge amount of work that if the load on it is too great, sooner or later it itself may need our help. Therefore, assessing the condition of our liver and nearby organs in time by undergoing a comprehensive ultrasound of the abdominal organs and kidneys with the adrenal glands means noticing alarming changes and starting the necessary treatment as early as possible!
What is jaundice
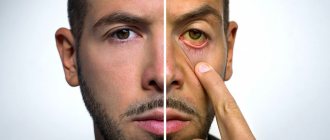
First of all, by jaundice we should not mean a specific disease (for example, hepatitis, as many people think), but a whole symptomatic complex that arises as a result of pathological processes in the liver and some organs. Essentially, jaundice is an excess amount of bilirubin in the body, which is externally manifested by the sclera, mucous membranes and skin becoming yellow.
Normally, bilirubin is formed in the liver and spleen from hemoglobin as a result of the breakdown of red blood cells, after which it is converted by the liver into bile and excreted from the body. With jaundice, the normal process of conversion and excretion of bilirubin is disrupted, so it remains almost completely in the blood, slightly excreted through the kidneys and skin.
People with:
- neoplasms in the liver;
- congenital anomalies of the bile ducts;
- pathological processes in the liver and gall bladder;
- the presence of parasitic organisms;
- postoperative complications;
- post-reaction to certain medications.
Jaundice of the newborn. Dangerous or not? How to treat jaundice?
Has your newborn's skin suddenly started to turn yellow? What is the reason and should I worry? Is it possible that this jaundice is a sign of liver damage?
So, what is neonatal jaundice?
Neonatal jaundice is a term used to describe the process of turning the skin, mucous membranes, and whites of the eyes (sclera) yellow in infants. The reason your baby turns carrot color is an increased level of the pigment bilirubin, which accumulates in the blood and cannot quickly leave it because the baby’s liver cannot cope.
This is a completely normal condition for most babies who have just been born; jaundice in newborns is not dangerous and in some cases goes away on its own over time, however, the level of bilirubin at this moment must be strictly monitored.
However, yellow skin color is not always so harmless. Jaundice is sometimes a sign of a dangerous condition, a threat to the health and even life of the baby.
When the level of bilirubin increases for a long time and/or to high numbers, kernicterus develops - a serious complication of any jaundice in newborns.
The pigment is toxic and affects nervous tissue. Negative effects of pigment on a child: can lead to neurological disorders, impaired speech development, retardation in physical or mental development, blindness or deafness.
Children at risk:
- Premature
- Having had an intrauterine infection
- Labor hypoxia
- Birth asphyxia
Other causes of jaundice in a baby may include the following factors:
- Reaction to mother's breast milk;
- Reaction to drugs;
- Various infections of mother and baby;
- Birth injuries;
- Diabetes mellitus in the mother;
- Congenital hepatitis, etc.
Types of jaundice
Depending on the reasons that caused jaundice, it is divided into forms:
- physiological (neonatal) - usually occurring in newborns (more often in weakened or premature infants) due to the adaptation of an immature enzyme system to new environmental conditions;
- parenchymal (liver) - usually occurring when the structure and function of liver cells (hepatocytes) are disrupted due to neoplasms and drug effects on the liver, or hepatitis or cirrhosis;
- hemolytic (suprahepatic) - usually occurring when red blood cells are destroyed and indirect bilirubin increases in anemia, lymphocytic leukemia, lymphosarcoma or tropical malaria;
- conjugation – usually occurring when the liver is exposed to provoking factors and congenital pathologies;
- mechanical (subhepatic) - usually occurring when direct bilirubin increases due to the inability to remove it through bile ducts blocked (by stones, tumors or helminths).
According to the duration of its course, jaundice is divided into:
- spicy;
- protracted;
- chronic.
Features of the disease
Jaundice in children in the first weeks of life is especially dangerous in the nuclear form, when, due to imperfections of the internal organs, poisonous indirect bilirubin affects brain cells, causing convulsions and, in especially severe cases, coma.
In 50% of cases, physiological jaundice is diagnosed in newborns - its causes are prematurity, increased utilization of the fetal form of hemoglobin, which are associated with pathology of intrauterine development. With early diagnosis of jaundice, consequences and dangerous complications can be avoided, the baby’s condition returns to normal, and the organs begin to function properly.
Symptoms of jaundice in an adult appear only due to serious disorders in the hematopoietic system or the development of diseases of the internal organs. It is necessary to establish the cause of the violation of bilirubin utilization. Diagnosis of jaundice includes laboratory and instrumental studies: ultrasound, MRI, CT and others.
Diagnosis of jaundice
Typically, the danger is not caused by jaundice itself, but by the pathologies that caused it. As a result of intoxication of the body with bilirubin, a serious failure of its various systems can occur, and in young children - mental retardation. Therefore, accurate diagnosis of this condition is so important, for which they carry out:
- comprehensive ultrasound of the abdominal cavity and retroperitoneal space;
- laboratory blood tests (general and biochemical blood tests);
- liver functional studies;
- liver biopsy.
Diagnostics
At the Moscow Clinical Hospital on Yauza, you can undergo rapid diagnostics of all types of hyperbilirubinemia within 1–2 days and begin treatment. Our doctors will conduct an examination and differential diagnosis, and prescribe treatment in accordance with modern medical standards.
The experience and high qualifications of doctors, modern equipment of the hospital, the location of all treatment and diagnostic units in one building will reduce the effort and time to make an accurate diagnosis and bring the patient closer to effective treatment.
The clinic has everything necessary to diagnose the causes of any type of increased bilirubin:
Laboratory tests : blood test for direct and conjugated bilirubin, liver enzymes, free iron, analysis of protein fractions, inflammatory and tumor markers, enzyme immunoassay of blood for all types of infections, etc.
Modern ultrasound and endoscopic diagnostics with tissue biopsy sampling and recording of the study on a digital medium. EndoUS is a combined method that allows one to identify a space-occupying formation in the wall of the digestive tract, the depth of its spread, and clarify the type of treatment required (conservative or surgical). Endoscopic examinations can be carried out in a state of sedation (medicated sleep).
Computed and magnetic resonance imaging of all organs and tissues using modern contrast methods. MR cholangiopancreatography.
Consultations with medical specialists. If hemolysis is established, the patient will be examined by a hematologist and will give his recommendations. Increased destruction of red blood cells will be indicated by anemia in the complete blood count, high serum iron levels and high free bilirubin levels.
What is hepatitis
Hepatitis is an inflammatory process in the liver under the influence of a provoking (in most cases viral) agent, causing damage to its tissues.
Today, hepatitis is considered one of the most common infectious diseases after ARVI, influenza and chickenpox. Most often, the disease is diagnosed in young people aged 15-30 years (especially those prone to unprotected sex and drug use), another “risk group” is usually represented by medical specialists who have direct contact with blood (including infected people).
Consequences of jaundice
In most cases, physiological jaundice goes away completely without causing any harm to the child. Consequences can develop only after pathological forms of jaundice - with insufficient or incorrect treatment. In such cases, children may be delayed in development and suffer serious damage to the nervous system.
Children who have suffered any form of pathological jaundice must be observed by a pediatrician and a pediatric neurologist!
The Healthy Family Clinic offers a rental service for a special phototherapy lamp, which is used to treat jaundice in newborns at home. Taking into account the need for special care and care for the newborn, the mobile device allows you to reduce the level of bilirubin without disrupting the baby’s daily routine. Unlike traditional equipment, modern technology has many advantages:
- Safety for the life and health of the baby: the combination of green and blue rays prevents overheating of the body and also does not have a negative effect on the child’s eyes;
- Compactness and mobility: the device weighs no more than three kilograms and has an ergonomic fiber-optic cushion, which allows you to transport equipment at home;
- Easy to use: the photo lamp has a timer and a safety thermostat, so it automatically controls the duration of the procedure and the intensity of radiation!
- All permits and certificates;
- Free delivery throughout Yekaterinburg! Delivery throughout the Sverdlovsk region is possible.
The basis for using a photolamp is the recommendation of a pediatrician. During an individual consultation, the doctor will determine the intensity, duration, and also establish a procedure scheme.
In addition, the baby’s parents can order an express test to measure bilirubin levels at home. A healthcare professional will help parents install and use the lamp correctly.
What are the symptoms of hepatitis
It must be remembered that the symptoms of hepatitis can be vivid, but sometimes they can be almost completely absent (giving time for the undetected disease to become chronic). However, quite often all types of hepatitis are characterized by common symptoms of any intensity:
- jaundice;
- change in urine color (darkening to brown)
- pain (often pressing) in the liver area;
- indigestion (nausea, vomiting with a bitter taste, diarrhea or constipation);
- weakness and increased fatigue;
- increased body temperature and headache;
- skin itching;
- increased liver size.
Hepatitis classification
In its form, hepatitis can be acute or chronic.
Depending on the provoking factor, hepatitis is divided into:
- infectious (caused by viruses or bacteria);
- toxic (when the body is poisoned with alcohol, chemicals or drugs);
- autoimmune (caused by autoimmune pathologies);
- radiation (for example, as a consequence of radiation therapy).
Viral hepatitis, in turn, is divided into types (depending on the virus that provokes the disease):
- hepatitis A (Botkin's disease) - transmitted through contaminated food and water, with an incubation period of 2-6 weeks, after the disease giving lifelong immunity to this type;
- hepatitis B - transmitted through unprotected sexual contact and through open access to blood (at home, dentistry, cosmetology, etc.) using unsterilized instruments, with an incubation period of 1.5-6 months, the duration of the acute disease is from 6 to 8 weeks (with recovery in 90% of cases) and rare transition to chronic;
- hepatitis C is the most dangerous type, transmitted in the same way as hepatitis B, but with almost unnoticeable symptoms, which is why the disease can proceed unnoticed by the patient for years in a chronic form, leading to cirrhosis and liver cancer;
- hepatitis D – transmitted in the same way as hepatitis B and C, but developing only after infection with the hepatitis B virus, easily becoming chronic and ending in cirrhosis of the liver;
- hepatitis E is transmitted in the same way as hepatitis A, with similar symptoms, usually common in African and Asian countries.
Publications in the media
Jaundice is a symptom of various diseases: yellow discoloration of the mucous membranes, sclera and skin, due to the deposition of bile pigments in them.
Classification • Suprahepatic • Hepatic (hepatocellular) • Subhepatic (cholestatic).
Bilirubin metabolism • Indirect bilirubin (unbound, unconjugated) is formed during the breakdown of Hb in the cells of the reticuloendothelial system (80%) and other heme-containing proteins (myoglobin, cytochromes, etc.) in the liver (20%) •• Indirect bilirubin is insoluble in water, lipotropic, not excreted by the kidneys, toxic, bound to albumin in the blood •• Liver cells absorb indirect bilirubin from the blood and conjugate it with glucuronic acids (using the enzyme uridine diphosphate glucuronyltransferase [UDPGT]) to form direct (bound, conjugated) bilirubin •• Direct bilirubin water-soluble, insoluble in fat, non-toxic, can be excreted by the kidneys (when circulating in the blood in high concentrations) •• Direct bilirubin is excreted in bile •• In the intestine, under the influence of bacterial enzymes, direct bilirubin is converted into urobilinogens, which give the characteristic color to stool. Urobilinogens are partially absorbed and enter the liver through the portal vein, where they are destroyed by hepatocytes to di- and tripyrroles. Through the middle and lower rectal veins, anastomosing with the inferior vena cava system, urobilinogens enter the systemic circulation and are then excreted by the kidneys •• In healthy individuals, total serum bilirubin is mainly represented by indirect bilirubin (no more than 20 µmol/l), direct bilirubin is not more than 25% of the total, the feces are colored, traces of urobilin are present in the urine.
ETIOLOGY
• Suprahepatic jaundice is caused by increased hemolysis of red blood cells •• Poisoning with substances that cause hemolysis (for example, snake venom, sulfonamides, arsenic hydrogen) •• Transfusion of incompatible blood •• Large hematomas •• Hemolytic disease of the newborn •• Autoimmune hemolytic anemia •• Hereditary hemolytic anemia ( microspherocytic anemia of Minkowski–Choffard, sickle cell anemia, thalassemia, etc.).
• Hepatic jaundice •• Damage to hepatocytes: infectious, toxic (drugs, alcohol) hepatitis, liver cirrhosis •• Low activity of UDPHT in newborns (transient jaundice of newborns) •• Hepatic jaundice can be hereditary ••• Impaired transport of bilirubin from hepatocytes to bile ( Dubin-Johnson syndrome) ••• Absence of UDFGT - Crigler-Nayar syndrome type I ••• Significant deficiency (less than 10% of the norm) UDFGT - Crigler-Nayar syndrome type II ••• Insufficient activity of UDFGT (Gilbert-Meulengracht syndrome).
• Subhepatic jaundice develops when there is an obstruction to the outflow of bile into the duodenum •• Stones in the bile ducts •• Cancer of the biliary tract and cancer of the head of the pancreas •• Parasitic lesions of the liver •• Atresia of the biliary tract.
PATHOGENESIS • All types of jaundice are united by one symptom - hyperbilirubinemia, on which the brightness of the skin color depends: from a light lemon tint to orange-yellow and green or olive-yellow •• Yellowing of the skin and sclera begins when the bilirubin concentration is more than 26 mmol/l • • Impregnation of the skin with pigment takes time: during experimental ligation of the common bile duct, hyperbilirubinemia increases after 24 hours, but the skin becomes colored only 5–8 days later • There are 4 main mechanisms for the development of jaundice •• Increased formation of indirect bilirubin (hemolysis) •• Impaired uptake of indirect bilirubin hepatocytes and its transport inside the hepatocyte •• Impaired conjugation of indirect bilirubin in hepatocytes •• Impaired excretion of direct bilirubin from the hepatocyte into the bile capillary or obstruction at the level of larger biliary tracts.
• Hemolysis •• The concentration of indirect bilirubin in the blood serum is moderately increased (usually 2-3 times), because. liver functions are not impaired •• The stool is very intensely colored (a lot of direct bilirubin is formed and it is excreted into the bile) •• The concentration of urobilin is increased in the urine (because urobilinogen is absorbed in large quantities through the rectal veins and filtered into the urine).
• Hepatitis •• In the blood serum, the concentration of indirect (impaired uptake, transport and conjugation) and direct (impaired excretion, destruction of hepatocytes, impaired outflow due to compression of the bile ducts in the portal tracts by inflammatory infiltrates) bilirubin is increased •• In most cases, the concentration is increased to a greater extent direct bilirubin (intrahepatic cholestasis); an increase in the concentration of indirect bilirubin indicates the predominance of necrosis of hepatocytes •• Feces are usually discolored, but may not be changed •• Urine is dark due to direct bilirubin (filtered into urine) and urobilinogen (not destroyed in the liver, enters the systemic circulation and is filtered into urine ).
• Cholestasis •• The concentration of direct bilirubin is increased in the blood serum •• The feces are discolored •• The urine is dark (due to the filtration of direct bilirubin into the urine), there is no urobilin in the urine (since direct bilirubin does not enter the intestine).
• Isolated disorders of conjugation or excretion of bilirubin are characteristic of hereditary syndromes. Pathomorphology in cholestasis • Bile pigment in hepatocytes • “Bile lakes” • Dilation of bile canaliculi • Signs of damage to the bile ducts • Formation of new bile ducts.
History • Compounded family history of anemia, any manifestations of liver and biliary tract diseases • Contact with patients with infectious hepatitis, stay in hepatitis endemic regions during the last 2 months, parenteral interventions, drug administration, casual sexual intercourse during the last 6 months • Working with hepatotoxic substances • Alcohol abuse • Treatment with hepatotoxic drugs • Biliary colic, cholelithiasis • Deterioration of general condition, weight loss.
CLINICAL MANIFESTATIONS
• Onset of the disease: from the prodromal period (intoxication syndrome, nausea, vomiting, dyspepsia - with infectious hepatitis), after biliary colic (with cholelithiasis), gradual (with tumors), after infection or hypothermia (with hemolytic anemia) • Jaundice with hemolysis dim, the patient is more pale than jaundiced, with obstruction the jaundice has a green tint, with hepatitis - with an orange tint (with cholestatic forms - with a green tint).
• Suprahepatic jaundice •• Splenomegaly predominates over liver enlargement •• Intense coloring of stool •• Manifestations of anemia.
• Hepatic jaundice •• Enlargement and hardening of the liver from the onset of the disease •• Skin itching is possible •• The spleen is sometimes enlarged •• In severe forms there may be manifestations of hemorrhagic syndrome, hepatic encephalopathy •• Feces are discolored at the height of the disease, urine is dark •• With chronic hepatitis and liver cirrhosis - extrahepatic signs (telangiectasia, hepatic palms), signs of portal hypertension, ascites.
• Subhepatic jaundice •• Skin itching, as a rule, is pronounced •• The gallbladder is enlarged and painless with tumors; in case of cholelithiasis, it may not be palpable, but a pain point is found in its projection •• The liver is enlarged •• Feces are discolored, urine is dark • • Signs of the underlying disease.
LABORATORY RESEARCH
• CBC • Liver function tests • Determination of direct bilirubin and urobilin in urine • Proteinogram • Reticulocyte count, determination of osmotic resistance of erythrocytes, blood smear examination, Coombs test, bone marrow puncture are indicated for suspected hemolytic anemia • Markers of viral hepatitis in hepatic jaundice.
• Suprahepatic jaundice •• The concentration of bilirubin in the blood serum is increased mainly due to indirect bilirubin •• Other indicators of liver function tests are not changed •• Reticulocytosis •• Osmotic resistance of erythrocytes may be reduced •• Possible changes in the shape and size of erythrocytes •• Signs of bone marrow irritation .
• Hepatic jaundice •• The concentration of bilirubin in the blood serum is increased mainly due to direct bilirubin •• The activity of ALT in the blood serum is significantly increased in acute hepatitis, slightly or moderately in chronic hepatitis •• In cholestatic forms of acute hepatitis, the concentrations of cholesterol, -glutamyl transpeptidase are increased , alkaline phosphatase •• In severe forms of acute hepatitis, liver cirrhosis, the albumin content, prothrombin index, and the results of the sublimate test are reduced •• The concentration of immunoglobulins and the results of the thymol test may be increased.
• Subhepatic jaundice •• The concentration of bilirubin in the serum is increased mainly due to the direct fraction •• The concentrations of cholesterol, alkaline phosphatase, g-glutamyl transpeptidase in the blood serum are significantly increased •• The activity of ALT in the blood serum is not changed, with prolonged cholestasis it is moderately increased •• PTI may be reduced, after the introduction of menadione sodium bisulfite it increases •• The concentration of a2- and b-globulins is increased.
INSTRUMENTAL STUDIES • Ultrasound, CT of the liver, biliary tract, pancreas allows you to diagnose obstructive jaundice, as well as identify an empty gallbladder (no mechanical obstructions) in the cholestatic form of acute viral hepatitis • Plain radiography of the chest allows you to identify tumors and their metastases • With FEGDS you can assess the condition of the major duodenal papilla and the possibility of bile outflow through it • Endoscopic retrograde cholangiopancreatography or percutaneous transhepatic cholangiography is indicated for questionable ultrasound results in cases where blockage of the extrahepatic bile ducts is suspected.
TREATMENT is determined by the etiology of the disease that caused jaundice - see Hemolytic anemia, Autoimmune hemolytic anemia, Sickle cell anemia, Acute viral hepatitis, Chronic viral hepatitis, Liver cirrhosis, Gallstone disease.
ICD-10 • P58 Neonatal jaundice due to excessive hemolysis • P59 Neonatal jaundice due to other and unspecified causes • D58 Other hereditary hemolytic anemias • D59 Acquired hemolytic anemia • A27.0 Leptospirosis icteric-hemorrhagic •• E80 Disorders of porphyrin and bilirubin metabolism • P55 Hemolytic disease of the fetus and newborn • B15 Acute hepatitis A • B16 Acute hepatitis B • B17 Other acute viral hepatitis • B18 Chronic viral hepatitis • B19 Viral hepatitis, unspecified
APPLICATIONS
Familial jaundice of newborns is a transient hereditary (r) form of hyperbilirubinemia, starting with jaundice 4 days after birth and developing due to a transient defect of glucuronyl transferase associated with the presence of inhibitors of its activity in the mother’s blood; may lead to bilirubin encephalopathy and cerebral palsy. Treatment: timely replacement blood transfusions and phototherapy. Synonyms: non-hemolytic transient jaundice of newborns, Lucea-Driscoll syndrome, Lucea non-hemolytic jaundice. ICD-10. P59 Neonatal jaundice due to other and unspecified causes.
Jaundice during breastfeeding (jaundice from mother's milk) is a spontaneously transient hyperbilirubinemia of unknown etiology in healthy children in the neonatal period. It can be early (appears within 3–4 days after birth) or late (within 4–5 days after birth) with maximum manifestations at 10–15 days. The maximum concentration of bilirubin can reach 20–30 mg% (340–510 µmol/l). No cases of bilirubin encephalopathy have been described. Diagnostic test: temporary cessation of breastfeeding for 24–48 hours. Treatment: phototherapy, phenobarbital, bilirubin adsorbents. ICD-10. P59 Neonatal jaundice due to other and unspecified causes.
Nuclear jaundice is a severe form of jaundice in newborns with a high concentration of unconjugated bilirubin in the blood, deposition of bilirubin in the basal ganglia and nuclei of the brain stem, occurring with severe impairment of brain functions. Etiology: excessive levels of indirect bilirubin in the blood (over 320 µmol/l in full-term infants and 150–250 µmol/l in premature infants). Causes of hyperbilirubinemia: incompatibility of mother and fetus by blood groups; hereditary spherocytosis, non-spherocytic hemolytic anemia, hemolysis caused by a lack of vitamin K3, taking nitrofurantoin, sulfonamide drugs, etc., hemorrhages, pyloric stenosis, Hirschsprung's disease; metabolic and endocrine disorders, obstructive disorders (Dabin-Johnson-Rotor syndrome, cystic fibrosis, tumors), sepsis, intrauterine infections, neonatal respiratory distress syndrome, severe fetal erythroblastosis. Clinical picture • Yellow-colored amniotic fluid • From birth, moderate jaundice, progressing hourly • Arterial hypotension • Motor restlessness, convulsions • Enlargement of parenchymal organs • Opisthotonus, drowsiness, poor sucking, distorted or absent Moro reflex; late manifestations (after 6 months of life): deafness, paralysis, mental retardation. Diagnosis, treatment, prevention, prognosis - see Erythroblastosis fetalis; additionally treat the underlying disease. Synonym: bilirubin encephalopathy. ICD-10. P57 Kernicterus.
Gilbert's syndrome (#143500, defects of the UGT1A1 UGT1A1 gene, 1q21 q23, B) is a benign unconjugated hyperbilirubinemia of moderate severity. Prevalence is 5–7%, the syndrome more often develops in males in adolescence • In the blood serum, the concentration of indirect bilirubin periodically increases to 17–85 µmol/l. Jaundice is not constant, it can appear or intensify after infections, fasting and decrease after taking phenobarbital (tests with phenobarbital and fasting are used in diagnosis). Liver function is not impaired, the histological picture is not changed. The prognosis is favorable, no treatment is required. Synonyms: Gilbert–Meulengracht syndrome, Meulengracht jaundice, congenital hyperbilirubinemia, constitutional hyperbilirubinemia, Gilbert–Lerbouyer syndrome. ICD-10. E80.4 Gilbert's syndrome
Crigler–Nayjar syndrome (type I, 218800, r; type II, 143500, Â) is a rare hereditary disorder associated with UDPG deficiency and manifested by unconjugated hyperbilirubinemia.
• Type I •• UDFGT activity is completely absent in the liver •• Very high concentration of indirect bilirubin in the blood serum, kernicterus develops •• Patients usually die in the 1st year of life •• Phenobarbital is ineffective, plasmapheresis has a temporary effect •• Phototherapy can reduce the concentration of indirect bilirubin is 2 times •• Encephalopathy (kernicterus) can develop at any time during the first 10–20 years of life •• Liver transplantation leads to normalization of bilirubin metabolism, the prognosis improves • Transplantation should be performed at a young age, before the development of kernicterus . • Type II •• UDFGT activity is reduced to 10% or lower compared to normal •• The concentration of indirect bilirubin is high, but usually lower than in Crigler-Nayjar syndrome type I •• Phenobarbital is effective •• Sometimes the combined use of phenobarbital and phototherapy is necessary • • Patients survive to adulthood.
Abbreviations: UDPGT—uridine diphosphate glucuronyl transferase. Synonyms: congenital non-hemolytic jaundice type I, non-hemolytic hyperbilirubinemia with kernicterus. ICD-10. E80.5 Crigler–Najar syndrome.
Dubin-Johnson syndrome (*237500, defect in the gene for the tubular transporter of organic anions CMOAT, 10q24 [*601107], r) is a hereditary pigmentary hepatosis caused by impaired transport of bilirubin from hepatocytes to bile due to a mutation in the protein gene responsible for the hepatobiliary transport of various organic anions; clinically manifested by jaundice with a moderate increase in the content of direct bilirubin in the blood and its appearance in the urine; During a liver biopsy, a dark, brown-orange pigment (lipochrome) is found in hepatocytes. Treatment: reduction of bilirubinemia with phenobarbital. Synonyms: Dubin-Johnson jaundice, non-hemolytic constitutional jaundice with lipochromic hepatosis, conjugative hyperbilirubinemia type II. ICD-10. E80.6 Other disorders of bilirubin metabolism.
Rotor syndrome (*237450, conjugated hyperbilirubinemia type I, r) is clinically similar to Dubin-Johnson syndrome; Unlike the latter, with Rotor syndrome there is no accumulation of pathological pigment in liver cells, oral cholecystography is often normal, and an increase in urinary excretion of coproporphyrin is noted. ICD-10. E80.6 Other disorders of bilirubin metabolism.
Cholestasis rare • Cholestasis with gallstones, ataxia and visual impairment (214980, r). Clinically: congenital cholestasis, gallstones, cerebellar ataxia, bilateral ptosis, retinal damage, optic nerve atrophy, camptodactyly, jaundice, prurigo. Laboratory: giant cell hepatitis according to the results of liver biopsy • Intrahepatic cholestasis with impaired metabolism of trihydroxycoprostanoic acid (*214950, r). Clinically: congenital jaundice, intrahepatic cholestasis, bile duct insufficiency. Laboratory examination: absence of bile acids in bile, detection of trihydroxyprostanoic acid in bile. Synonym: alligator defect. Note. Typically, bile acids are synthesized in the liver by hydrogenation and hydroxylation of the steroid core of cholesterol with oxidation of the side chains. In some lower vertebrates, side chains are oxidized without hydroxylation (in alligators, trihydroxycoprostanic acid is the main component of bile) • Progressive intrahepatic cholestasis type 2 (*601847, 2q24, defect in the PFIC2, r gene) is a form of severe cholestatic liver disease; manifests in infancy with intermittent jaundice and cholestasis and rapidly progresses to end-stage liver failure and death in childhood. Clinically: progressive familial intrahepatic cholestasis, intermittent jaundice.
What is liver cirrhosis
Liver cirrhosis is a pathological and chronic process in the liver, as a result of which its parenchymal tissue is replaced by fibrous connective tissue (stroma). There is also a structural restructuring of the vascular bed and a decrease in the number of normally functioning hepatocytes (liver cells).
According to statistics, the global annual mortality rate from cirrhosis is about 300 thousand people, with a progressive upward trend. The disease most often affects men over 40 years of age, those prone to alcoholism, as well as patients with:
- chronic hepatitis B, C and D;
- pathologies complicated by fatty hepatosis;
- some hereditary diseases (for example, hemochromatosis);
- some autoimmune diseases;
- toxic liver damage from chemicals.
Consequences and prognosis for obstructive jaundice
The prognosis will be favorable in cases where the treatment of jaundice was timely and correct. The behavior of the patient himself is also of great importance. If you adhere to the principles of proper nutrition and strictly follow all the doctor’s instructions, the risk of relapse or complications will be minimal. Otherwise, the likelihood of recurrent obstructive jaundice will be very high. In addition, the risk of developing concomitant diseases, for example, liver failure, liver cirrhosis, encephalopathy, sepsis, etc., will increase.
What are the symptoms of cirrhosis
Symptoms of cirrhosis may be completely absent for quite a long time, or appear slightly. Most often, the disease can begin to manifest itself:
- increased fatigue and decreased mental activity, weakness and irritability;
- indigestion (a feeling of bitterness in the mouth, nausea and vomiting, flatulence and upset stool), especially in the morning;
- pain in the right hypochondrium (increased after drinking alcohol or fatty foods, as well as during physical activity);
- increased bleeding in the mucous membranes and subcutaneous hemorrhages (with characteristic spider veins at the top of the body and redness of the palms);
- itchy skin and aching joints.
A long-term progressive disease is also characterized by:
- decrease in body weight and muscle volume;
- “protrusion” of the abdomen (against the background of thinning limbs with thickening fingertips) with an enlarged liver and spleen, ascites;
- painful swelling of the joints;
- jaundice;
- decreased sexual function and secondary sexual characteristics.
Consequences of jaundice syndrome, prevention
With proper and timely treatment, jaundice can be completely cured. The exception is advanced cases, which will result in disruption of the gallbladder and liver. A terrible consequence of jaundice syndrome in children is developmental delay.
Preventive measures are aimed primarily at preventing diseases that cause jaundice.
Let us remember that jaundice is a fairly common disorder and can accompany various diseases. If jaundice of the skin and pain in the right hypochondrium are detected, it is necessary to urgently seek medical help. Only timely treatment will help cope with the disease and avoid negative health consequences. Sign up for a consultation now.
Diagnosis of cirrhosis
Diagnosis of the disease is based on the results of a comprehensive examination of the condition of the liver and organic systems most closely related to its work, as well as establishing the causes of cirrhosis. To do this:
- comprehensive ultrasound of the abdominal organs and retroperitoneal space (kidneys and adrenal glands), as well as portal vessels;
- laboratory blood test (including biochemical, for the presence of hepatitis viruses, as well as a coagulogram);
- esophagogastroduadenoscopy to identify dilated veins of the esophagus;
- liver biopsy and scintigraphy.
Possible causes of parenchymal jaundice
Parenchymal jaundice can be provoked by various pathological conditions that disrupt the ability of hepatocytes to capture, bind and convert bile into bilirubin. The disease can be either congenital or acquired. Among the main causes of parenchymal jaundice are the following factors:
- Infectious hepatitis
. Hepatitis A, B, C, D, E can provoke the death of hepatocytes. This occurs due to the indirect cytotoxic effect of these viral pathogens. Parenchymal jaundice can also be caused by herpetic, adenoviral or enteroviral infections, infectious mononucleosis, sepsis, leptospirosis; - Toxic influence
. Various hepatotropic poisons can destroy liver tissue and provoke parenchymal jaundice. These include oxidizing agents based on nitrogen oxides, hydrazine, chloroethane, ethylene glycol. Alcohol also has a toxic effect on the liver; - Degeneration of hepatic parenchymal tissue
. Due to fibrosis, cirrhosis of the liver, sclerosing cholangitis, the functional tissue of the liver is replaced by connective tissue. It also occurs in liver failure, hepatocellular carcinomas, and other forms of primary liver cancer; - Autoimmune damage to hepatocytes
. This happens due to an increase in the titer of autoantibodies. It can be provoked by rheumatoid arthritis, Sjogren's disease, glomerulonephritis, autoimmune thyroiditis; - Intrahepatic cholestasis
. The cause of destruction of hepatocytes may be a violation of the permeability of liver membranes. This is typical for pregnant women, patients with cholestasis, cholestatic hepatitis, cystic fibrosis; - Hereditary diseases
. Parenchymal jaundice can also occur as a congenital defect. Most often, this form is diagnosed with Gilbert, Crigler-Nayyar, Dabin-Johnson, Rotor syndrome; intrahepatic disorders. Parenchymal jaundice can be provoked by ischemia and endotoxic changes in the liver, heart failure, transfusions, the consequences of surgical interventions, parenteral nutrition, and prolonged fasting.
Treatment of cirrhosis
Typically, treatment of liver cirrhosis is aimed at stopping (in the initial stages of the disease) or slowing down progressive pathological processes. Conservative therapy is strictly individual and often consists of:
- taking medications (hepatoprotectors);
- following a diet (with the obligatory exclusion of alcohol, fatty and canned foods);
- excluding physical and emotional overload.
Treatment of end-stage cirrhosis can only be associated with liver transplantation.
It must be remembered that only a preventive comprehensive ultrasound of the abdominal organs in most cases can help to recognize pathological changes in the liver in time, even before the first symptoms appear! Save your health!
Principles of treatment of obstructive jaundice
The main objectives when drawing up a treatment plan are the elimination of cholestasis (stagnation of bile) and the prevention of liver failure. To do this, the doctor draws up a comprehensive program, which can include both conservative and surgical methods.
Diet for obstructive jaundice
It is necessary to follow certain nutritional rules both before the main treatment and after its completion. Patients with obstructive jaundice are advised to maintain a drinking regime, as water accelerates the excretion of bilirubin, thereby reducing its negative effect on the body. It is also very important to completely avoid alcohol, very fatty and fried foods, mayonnaise, sauces, and hot seasonings. Food should be consumed in small portions 5-6 times a day. In this case, it is necessary to monitor the temperature of the dish. It shouldn't be too hot or cold. The best option is warm food, as it helps regulate the secretion of bile, which is especially important for obstructive jaundice.
Other general recommendations regarding diet include limiting the amount of salt in the diet. It is known that excess salt contributes to fluid retention in the body, causes swelling and makes it difficult to remove harmful substances from the body. Patients with obstructive jaundice are recommended to consume no more than 4 grams of salt per day. In general, the exact nutrition plan, calorie content and composition of dishes are selected individually for each patient, taking into account his preferences. There are lists of permitted and prohibited foods, as well as those foods that should be limited. It is these lists that the doctor is guided by when drawing up a nutrition program. For example, permitted products include:
- Vegetables (carrots, cucumbers, cabbage, tomatoes, broccoli).
- Bananas and apples.
- Dried fruits.
- Various porridges (buckwheat, oatmeal, pearl barley).
- Bran bread, pasta, crispbread.
- Jam, honey, marmalade.
- Lean meat (rabbit, beef), poultry (chicken breasts, turkey fillet) and fish (pollock, hake).
- Fruit juices and tea.
A diet for obstructive jaundice involves the complete exclusion of canned vegetables, legumes, grapes, baked goods, white bread, full-fat milk, cream, fatty meats and fish, smoked meats, carbonated drinks, coffee, and animal fats.
Drug treatment
Drug therapy for obstructive jaundice is prescribed to reduce the severity of symptoms, prepare the patient for surgery and reduce the risk of complications. The extent of medical care largely depends on the degree of jaundice. For example, in severe cases, drug treatment is carried out in an intensive care unit and includes:
- Massive infusion therapy.
- Forced diuresis.
- Vitamin therapy.
- Hepatoprotectors.
- Amino acids.
- Metabolism stimulants.
- Hormonal drugs.
To relieve symptoms, in mild forms of obstructive jaundice, antispasmodics, enveloping drugs, antacids and other medications can be prescribed.
Surgery
Surgical treatment is the only effective method that allows you to restore the patency of the bile ducts and thereby eliminate the cause of obstructive jaundice. All known types of operations can be divided into two groups: minimally invasive techniques and direct operations.
Minimally invasive methods of surgical treatment
This group of methods is highly effective and low-traumatic, but it is impossible to apply them to all patients in a row due to certain limitations. Minimally invasive treatment of obstructive jaundice is carried out using endoscopic techniques and percutaneous transhepatic cholangiostomy. Endoscopic operations can be of the following types:
- Endoscopic papillosphincterotomy and lithoextraction.
- Local lithotripsy and lithoextraction.
- Bougienage and stenting of the bile ducts.
In these cases, to treat obstructive jaundice, a gastroduodenoscope with special instruments is used that allow crushing and removing stones, installing stents, and removing tissue. Endoscopic operations in most cases are performed without general anesthesia and do not require long recovery time.
Percutaneous transhepatic cholangiostomy is used in cases where it is impossible to perform decompression of the biliary tract using a gastroduodenoscope. The essence of the operation is to install a drainage tube under ultrasound or x-ray control. In this case, the skin, muscles of the anterior abdominal wall and liver tissue are pierced with a special puncture needle. In the future, the drainage tube can be used not only to drain bile, but also to introduce antibacterial or other drugs directly into the bile ducts.
Direct surgical interventions allow you to create full access to the gallbladder and eliminate obstructive jaundice of any complexity. The surgeon can perform anastomoses, install stents, and perform reconstructive operations. The intervention can be performed using laparoscopic instruments or the classic open cavity method. The latter option is the most traumatic, requires long-term rehabilitation and is accompanied by an increased risk of complications, so it is used only in the treatment of complex cases of obstructive jaundice.
General principles of treatment of obstructive jaundice
Generally speaking, the treatment tactics for obstructive jaundice include two stages. At the first stage, conservative therapy and minimally invasive methods of surgical treatment are prescribed. It is recommended to carry out such treatment in the first 2-3 days from the moment the patient is admitted to the hospital. If these methods are ineffective, then move on to the second stage of treatment of obstructive jaundice, which involves more radical methods. Treatment at the peak of jaundice is associated with a high risk of developing postoperative complications, so it is carried out only if there are vital indications.
Other treatments
Effective treatment of jaundice involves eliminating the underlying disease that led to the development of this symptom. To do this, it is necessary to use either conservative or surgical methods. Other treatment options for obstructive jaundice, in particular traditional medicine, home treatment and self-medication will not help achieve the desired result. For a certain period of time, they will help hide the symptoms and alleviate the patient’s condition, but the main process will continue to progress and lead to the development of complications. Therefore, when the first signs of obstructive jaundice appear, it is necessary to seek qualified medical help, which will help radically solve the problem.
“Physiological jaundice” of newborns
Physiological jaundice occurs in approximately 60% of newborns.
The reason for the increase in bilirubin in the blood of newborns is accelerated hemolysis (decomposition) of red blood cells due to the functional “immaturity” of the liver in the first days of life. Physiological jaundice is a transient condition, appears, as a rule, on the third day, gradually intensifies by the fifth, and slowly disappears by 2-3 weeks of the child’s life.
Increased bilirubin in newborns and “physiological” jaundice are in most cases safe, do not require treatment and do not leave consequences for the child.
Prevention
You can protect yourself from parenchymal jaundice if you do everything possible to prevent the diseases that cause it. Doctors recommend following the following rules:
- Do not self-medicate - take any medications only after consultation with a specialist;
- Avoid drinking alcoholic beverages;
- Avoid exacerbation of chronic diseases;
- Maintain personal hygiene measures;
- Monitor your body weight;
- Lead a healthy and active lifestyle;
- Eat properly and balanced;
- Observe safety precautions when working with chemicals;
- Get blood and urine tests and an abdominal ultrasound every year.
If you suspect signs of parenchymal jaundice or are trying to get rid of it, be sure to contact the Medscan medical center. Experienced doctors will prescribe the necessary examination and develop an individual treatment plan. With them you can get rid of parenchymal jaundice and minimize the risk of possible complications.