Thrombophlebitis (TF) is an inflammatory process that affects the wall of venous vessels, resulting in the formation of blood clots. Depending on the stage of development, several types of the disease are distinguished.
Signs of the development of pathology are an increase in body temperature, redness and thickening in the area of the affected vein, pain, etc. These symptoms should be the reason for mandatory contact with a specialist who will conduct an examination and identify the cause of these symptoms.
Medical offers its clients high-quality and professional assistance from a phlebologist in the diagnosis, treatment and prevention of vein diseases, including varicose veins. In the clinic, equipped with modern equipment and equipment, you can receive high-quality services from experienced doctors at reasonable prices.
What is venous thrombophlebitis?
The disease is an inflammatory process that takes place in the venous wall, and is accompanied by the formation of blood clots (thrombi), which have different densities and close the lumen of the vein. As a result, partial or complete blockage of blood vessels occurs.
The pathology has an acute and chronic form, and can occur in superficial and deep veins. TF is most often diagnosed in the lower extremities, but it can also affect the venous vessels of any other parts of the body. If therapy is not carried out correctly and on time, it can cause undesirable consequences, including:
- purulent abscess;
- blood clot separation;
- blood poisoning.
Thrombophlebitis of the superficial veins has more severe symptoms compared to the disease affecting the deep veins. However, in both cases, timely diagnosis is very important, which will allow you to begin treatment without wasting time, and thereby avoid worsening the situation.
Treatment with leeches
In acute thrombophlebitis of the lower extremities, leech therapy is practiced. They are dispersed in the direction of the affected vein, up to a maximum of 10 pieces. for 1 time. And not on the vein itself, but at a distance of at least 1 cm from it, staggered. in a checkerboard pattern, if leeches are placed in quantities of up to 10 pieces along the painful vein in a checkerboard pattern at a distance of at least 1 cm from the vein. Up to 60 leeches can be delivered per course.
The use of leeches is not suitable for everyone and not always. Minor reactions are also possible - redness, swelling of the skin, itching. This is an allergy to bites, but it is not serious and will go away on its own fairly quickly. Hyperpigmentation rarely occurs. But in case of individual intolerance, Quincke's edema is possible.
Types of thrombophlebitis of the lower extremities
Depending on the affected area, the following types of thrombophlebitis of the lower extremities are distinguished:
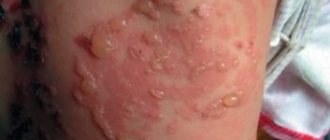
- TF of the superficial veins begins with the appearance of mild pain in the skin located along the saphenous veins. The skin changes its hue to red and becomes inflamed, its temperature rises. Also, in some cases, there is a slight increase in the temperature of the whole body, which remains elevated for about 6 days. Symptoms of this type of pathology include swelling of the limb in which a blood clot has formed. Condensed areas of various sizes may appear on it, which can be easily palpated. Painful sensations appear while walking.
- Deep vein TF, manifestations of which occur only when the blood clot enlarges. If a blood clot breaks off, chest pain, shortness of breath, and expectoration of blood occur. The development of pathology is indicated by swelling, pain during movement, and a change in the shade of the skin to bluish.
The severity of the disease is determined by the size of the filling and its location in the body. Symptoms are completely absent if there is no blockage of the vessel. This makes it much more difficult to identify the problem in a timely manner.
Septic thrombophlebitis of veins is also distinguished. It occurs due to purulent melting of a blood clot and transmission of infection through the bloodstream.
Based on characteristics such as the location of the affected area, TFs are distinguished:
- upper and lower extremities;
- vessels of internal organs.
Pathogenesis of the disease
Thrombophlebitis and phlebothrombosis develop according to a simple pattern. First, there is a sharp decrease in blood flow, then the damaged vascular endothelium provokes the release of interleukins (they are responsible for platelet aggregation), while simultaneously increasing their adhesiveness. As a result, blood clots form - pathological blood clots that attach to the walls of veins, arteries and even in the cavity of the heart.
Depending on the type of blood clots, thrombosis is distinguished:
- Parietal - a blood clot is attached to the wall of the vessel, but most of the lumen is preserved. This phenomenon is typical not only for thrombophlebitis, but also for some other diseases (aneurysm of the heart, blood vessels, chronic heart failure, etc.). In the case of mural thrombosis, one part of the thrombus is attached to the wall of the vein, and the other hangs freely into the lumen. With an increase in the speed of blood flow, small oscillatory movements, or awkward getting out of bed, such a clot can break off and provoke a pulmonary embolism.
- Obstructive (occlusive) - complete closure of the lumen by a thrombus is noted, as a result of which blood stops circulating through the affected area of the vein or artery. In this case, the patient must be treated urgently, as there is a risk of gangrene or death.
The thrombus-forming process can progress and lead to the enlargement of veins to impressive sizes. The location of the thrombus occurs along the length of the bloodstream. In the first few days, the clot is weakly fixed on the surface of the vessel. On days 5-6, it becomes more securely attached to the inner wall, which is why it begins to become inflamed.
Within 6 months, 70% of patients experienced an improvement in venous patency. In other cases, damage occurs to the vessels supplying the vein wall. This process is accompanied by gross fibrinous changes in the walls and disruption of the venous valves. As a result of the pathological process, there is a significant increase in pressure in the veins of the lower leg, and the general clinical picture is accompanied by the development of chronic venous insufficiency.
Reasons for education
Blood clots stick together much faster in the area where the pathological lesion occurred. This provokes a more rapid narrowing of the lumen and disruption of tissue nutrition. Key factors contributing to the development of the disease include:
- excess weight;
- lower limb injuries;
- varicose veins;
- incorrectly administered injection;
- the presence of tumors in the digestive system;
- low level of physical activity;
- previous operations;
- pregnancy;
- prolonged stay in an uncomfortable position;
- alcohol abuse and smoking;
- hormonal treatment and contraception;
- autoimmune processes.
Women are at higher risk of developing the disease due to high estrogen levels. It has also been proven that COVID-19 in 70% of cases causes an overreaction of the immune system, which causes a large number of blood clots to form.
Why does the disease occur?
Often the pathological process is triggered by the presence of several factors, which are called “Virchow’s Triad”:
- increased blood clotting (indicator significantly exceeds the norm) - the result of an excess/lack of blood clotting inhibitors, a protein with anticoagulant properties;
- poor condition of the walls of the vascular system (the structure at the cellular level is disrupted);
- phenomena of stagnation, accompanied by a slowdown in blood flow.
The etiology of thrombophlebitis also often involves:
- narrowing/expansion of blood vessels in the area of varicose nodes;
- slowdown of metabolic processes;
- dysfunction of hematopoiesis.
The listed pathological changes in the body, which cause vascular thrombophlebitis, do not arise out of nowhere. The etiology of phlebitis may be associated with:
- excess body weight;
- genetic predisposition to varicose veins, phlebothrombosis;
- sedentary lifestyle;
- dehydration and insufficient fluid intake;
- treatment with medications that negatively affect blood clotting;
- pregnancy, childbirth;
- nicotine addiction;
- injuries of the lower extremities;
- cardiovascular diseases;
- surgical intervention not only on the lower extremities, but also in the peritoneum and pelvic organs;
- age-related changes in the walls of blood vessels (elasticity decreases, blood viscosity increases);
- infectious and purulent-septic infectious processes;
- hypothermia;
- allergies;
- acquired problems with blood clotting;
- malignant tumors.
Also, the risk of developing phlebitis increases if there is information in the medical record about a heart attack, stroke, large blood loss and complications of the postpartum period. The risk group includes people who lead a sedentary lifestyle, suffer from arterial hypertension or have a weakened immune system.
Symptoms and signs of thrombophlebitis
Symptomatic signs of TF vary depending on the form of its course. In the case of acute pathology, its symptoms appear within the first two weeks. The subacute form is characterized by the manifestation of symptoms within a month.
If we are talking about TF of the superficial veins, then its signs are painful sensations when palpated, redness of the skin in the affected area, and the appearance of a clear venous pattern. TF of the deep veins is characterized by swelling. Symptoms also include:
- difference in temperature between healthy and affected areas;
- pain that increases with exercise;
- tissue tension;
- chills, etc.
Among the symptoms of the disease, there are also those that can only be detected during medical diagnosis. This:
- decreased blood circulation rate;
- thickening of vascular walls;
- occlusion;
- valve dysfunction;
- increased blood viscosity.
Thrombophlebitis, the symptoms of which are described above, requires urgent medical intervention if the swelling and pain are pronounced, and there is also fever or shortness of breath, accompanied by coughing attacks and spasms in the chest. These symptoms indicate an increased risk of blood clots breaking off and subsequently entering the lungs, which will lead to death.
Signs of acute thrombophlebitis
Acute thrombophlebitis is manifested by painful sensations in the leg where the veins are affected. Pain is felt on the skin along the inflamed area of the vein. This area can be felt like a painful cord, possibly with nodes. There is swelling of the skin around it with redness. The swelling becomes more noticeable during the day during exercise, and subsides during the night.
Hyperthermia is observed - the inflamed area of the skin becomes noticeably warmer. Body temperature can reach 37.5-38°C, and in case of infection - up to 39°C. Chills are possible. After some time, the body temperature drops to normal or remains only slightly elevated. However, it happens that thrombophlebitis develops without fever.
The general condition is marked by loss of strength, rapid fatigue, even with minor physical activity. When walking, the pain in the leg intensifies.
Diagnostics
To diagnose the disease, you should contact a qualified specialist. He will conduct an examination and prescribe additional measures to study the patient’s condition, including:
- Ultrasound;
- phleboscintigraphy;
- angiography;
- phlebography.
Any experienced phlebologist will suspect TF already during a visual examination, during which he will detect dense and painful nodes located under the skin of a red tint. However, to accurately confirm the diagnosis, an ultrasound examination of the veins in the legs should be performed. This method will allow the doctor to examine thrombotic masses in the lumen of the vein and assess the degree and nature of thrombosis.
After examining the patient, the phlebologist receives data that will help him prescribe appropriate therapy. Yuzhny MC specialists conduct research using modern equipment from trusted manufacturers, which, combined with their qualifications, allows them to accurately identify the disease and begin its treatment.
Which doctor should I contact?
If there are clear signs of the development of TF or other vascular diseases (varicose veins, gangrene, thrombosis, tropical ulcers, etc.), you should consult a phlebologist. His competence includes examining the patient in order to make a diagnosis and subsequently prescribe treatment. You can also contact a specialist in this profile to receive clarification on preventive measures.
You can make an appointment with a phlebologist at a medical clinic, where experienced specialists work who have confirmed their qualifications with many years of successful experience in identifying and eliminating diseases of the venous system. The clinic is equipped with the latest technology, which allows diagnosis and treatment to be made even more efficiently and quickly.
How is thrombophlebitis diagnosed?
A phlebologist is able to determine and prescribe adequate treatment for venous thrombosis of the lower extremities. In especially severe cases, consultation with a vascular surgeon is required. To diagnose this disease, in addition to visual examination and entering data into the patient’s medical record, they can use:
- Duplex ultrasound angioscanning using color Doppler mapping allows you to determine thrombosis localized below the level of the inguinal ligament. Shows the condition of the vessels, features of the movement of blood flow, thanks to which it is possible to determine the places of blockage and parietal thickenings.
- X-ray contrast venography - a contrast agent is injected into the venous system. This method is often used when the previous research is unreliable. Phlebography is especially good at identifying clots in the groin area.
- Magnetic resonance imaging (MRI) and magnetic resonance angiography (MRA) - allow you to examine peripheral and central veins. MRI is used to visualize blood clots, and MRA is used to visualize blood vessels.
- Radionuclide scintigraphy is the filling of a vein with a radioactive drug, the movement of which through the deep veins is monitored using a gamma camera. The method allows you to determine the speed and nature of blood flow. This technology is used in extremely difficult cases.
- Plethysmography is a study that is most widespread in Western countries. It is used to measure the degree of blood filling of the venous trunk during physical activity and rest. As a result, it is possible to determine the difference in the electrical resistance of the limb.
The use of laboratory tests is additional. They are not able to give a complete picture of the boundaries of the spread of phlebitis and thrombosis.
Great importance is given to differential diagnosis, which makes it possible to exclude other diseases and pathological conditions that have a similar clinical picture to thrombophlebitis:
- cellulite - subcutaneous fat tissue is affected, mainly in the lower extremities, accompanied by frequent cramps, changes in skin color, and dryness;
- lymphedema - depending on whether the disease is primary or secondary, it affects one or two limbs, is characterized by swelling of the lower leg, pain, fatigue;
- compression of the vessel by neoplasms or inflamed lymph nodes;
- stretching, rupture of muscle tissue - intermuscular hematoma puts pressure on the venous trunks, causing them to narrow;
- rupture of Baker's cyst - diagnosis is carried out using ultrasound.
Treatment of thrombophlebitis
The treatment regimen for thrombophlebitis is determined by the doctor based on the results of the patient’s examination and the stage of development of the disease. Today, both conservative treatment and surgical intervention are used to combat pathology. Only the attending physician has the authority to prescribe a particular therapeutic method.
At the present stage of development of medicine, pathology therapy does not necessarily involve a complex surgical operation. In some cases, it is possible to treat a person on an outpatient basis by taking medications prescribed by a phlebologist. At the same time, it is important to avoid any amateur activity in prescribing drugs in order to avoid aggravation of symptoms.
Some patients may be advised to wear compression stockings and elastic bandages if their general condition allows it. Drug treatment sometimes includes anticoagulants and anti-inflammatory drugs.
Operation
Surgery for TF is indicated in the following cases:
- the presence of signs of disease in the proximal part of the veins;
- combination of pathology with damage to the superficial vascular network;
- localization of the disease in the distal part of the vessels (does not require urgent surgical intervention, a planned operation is performed);
- thrombophlebitis of the deep veins of the lower extremities. In this case, the operation is prescribed taking into account the characteristics of the individual’s body.
In modern surgical practice, several types of operations are used to eliminate TF. Despite their differences, each type guarantees a good result. Popular techniques include:
- Crossectomy. During this type of operation, pathological areas of blood vessels are crossed in the area of the saphenofemoral junction.
- Stitching of the vena cava of the lower limb, which is carried out to narrow its lumen. This will not interfere with normal blood circulation, but will prevent it from carrying a large clot.
- Installation of a vena cava filter in the vein that supplies the leg. It is a design whose purpose is to retain large blood clots in order to prevent them from entering the general bloodstream.
- Endovascular method of catheter thrombectomy. It is carried out to completely remove clots from the lumen of deep veins and regenerate their patency. This leads to improved blood circulation and a reduced risk of progression of pulmonary embolism.
Laser treatment
The disease has been successfully treated for many years using laser. This technique, which allows you to relieve inflammation, pain and swelling, is carried out a day or two after the exacerbation subsides and is one of the most common today.
Laser treatment of the disease involves inserting a special device into a vein. It produces a temperature effect that leads to sealing of the damaged vein and stops the process of formation of blood clots in it. The main advantage of the manipulation is that it can be performed on an outpatient basis and there is no need to make surgical incisions on the skin.
Conservative
Conservative therapy for TF can only alleviate the symptoms of the disease. However, it is not effective in completely eliminating the threat of dangerous complications due to its inability to radically solve the problem.
This treatment includes:
- Consumption of non-steroidal medications that have an anti-inflammatory effect and relieve pain.
- Mandatory elastic compression. It is recommended to choose stockings over bandages.
- Local therapy, which includes ointments and creams containing non-steroidal anti-inflammatory components.
- Anticoagulant treatment involves taking medications that thin the blood and reduce inflammation.
Physiotherapy
Thrombophlebitis, after the removal of the acute inflammatory process, is also subject to treatment with physiotherapeutic techniques. Physiotherapy as a method of combating thrombophlebitis is prescribed for the purpose of:
- suppression of blood clotting;
- slowing down the development of the process of sclerosis of veins;
- eliminate inflammation;
- hemodynamic regeneration;
- reducing pain.
The main physiotherapeutic techniques include:
- UHF treatment;
- infrared laser therapy;
- CHUV irradiation with erythemal doses;
- high-frequency magnetic therapy;
- electrophoresis with the use of medications that have an anti-inflammatory effect;
- applications of paraffin and ozokerite.
Contraindications to physiotherapy in the treatment of acute thrombophlebitis are:
- The patient's body temperature rises above 38 degrees.
- Purulent processes in the body.
- Ischemic thrombophlebitis.
In order to exclude the possibility of developing thromboembolism, it is prohibited to use TF in therapy:
- Magnetotherapy with a “running” magnetic field.
- Vibration therapy.
- Low frequency electrotherapy.
- Pulsed magnetic therapy.
Vaccinations
People with acute TF should refrain from vaccination against coronavirus infection. If at the time of vaccination a person does not have an exacerbation of the chronic form of the disease, then there is no need to fear the formation of blood clots under the influence of vaccination.
It is worth considering that infection with COVID-19 increases the risk of blood clots and an extremely undesirable outcome. In this regard, patients suffering from TF are recommended to undergo vaccination against coronavirus.
Today, there are rare cases of complications occurring after vaccination in the form of blood clots. However, both domestic and foreign recommendations for the use of vaccines do not include a tendency to blood clots among the contraindications. Therefore, it is appropriate to say that the risks of contracting COVID-19 are much higher than the rare complications that arise during the post-vaccination period.
Traditional methods
Treatment of the disease with folk remedies should be auxiliary in nature and used only with the approval of the attending physician. It can give positive results only at the initial stage of development of the pathology, but it is not effective in its advanced form. Folk remedies are indicated to prevent the development and possible complications of TF.
Discussion of traditional methods of treatment with a doctor is mandatory if a person does not want to worsen the situation. The fact is that some alternative medicine recipes include plants that stimulate the functioning of the adrenal glands and are contraindicated in patients suffering from hypertension.
Drug treatment
It consists of prescribing anticoagulants, angioprotectors, non-steroidal anti-inflammatory drugs, and certain enzyme preparations. And antibiotics in case of acute purulent thrombophlebitis.
Special ointments are also used: Heparin, Essaven-gel, Ketonal 5% cream, Lyoton-gel and some others. Ointments such as Levomekol, Levosin and others, intended for the treatment of superficial skin lesions and ulcers, only worsen the problem.
Surgery is prescribed when the possible development of pulmonary embolism is suspected after differential diagnosis. Also, the surgical method gets rid of blood clots that have accumulated during acute thrombophlebitis in the bed of the great saphenous vein. The main indication for surgical treatment is signs of movement of part of the clot noticed during ultrasound.
Who is at risk?
The risk group for developing the disease includes the following categories:
- Pregnant women, women after childbirth and on hormone replacement therapy.
- Patients with a malignant tumor.
- Women who have been using contraceptives for a long time.
- Patients with excessively limited physical activity.
- Patients with pathologies of the venous system.
The likelihood of developing the disease is also high for people:
- Over the age of 60.
- With a previous stroke and episodes of TF.
- Smoking abusers.
- Suffering from obesity.
It is worth remembering that regular physical activity and giving up bad habits stimulate normal blood circulation, which will avoid the formation of blood clots. People who are included in one of the above risk groups should contact a phlebologist for an examination and recommendations for preventive measures.
Risk factors for the development of thrombophlebitis
- pregnancy, childbirth, gynecological operations (including abortions).
- varicose veins;
- prolonged bed rest (for example, after surgical and orthopedic operations);
- infectious diseases;
- stroke leading to paralysis of the limbs;
- motionless body position during a long trip by car or plane;
- obesity;
- oncological diseases (including surgical treatment of malignant neoplasms, radiation therapy and chemotherapy);
- dehydration;
- the use of hormonal contraceptives and other sex hormone preparations for the purpose of replacement therapy;
- increased blood clotting (hyperhomocysteinemia, antiphospholipid syndrome, etc.);
- puncture and/or venous catheterization.
The more risk factors a patient has, the higher the risk of developing thrombophlebitis.
If you have one or more factors from the above list, consult a specialist about methods of preventing venous thrombosis.
Complications of thrombophlebitis
Thrombophlebitis, the treatment of which is ignored or carried out incorrectly, can cause a number of complications. If we are talking about pathological damage to the superficial veins, then serious complications are rare. But they cannot be ignored because of the damage they can cause to health:
- Sepsis.
- Streptococcal lymphangitis.
- Spread of infection in the subcutaneous tissue.
- Change in skin color over the affected vessel.
- Thromboemolia of the pulmonary artery.
- Deep vein thrombosis.
The situation is more serious with the development of deep vein disease. In this case, the following complications are possible:
- Stroke or heart attack for patients with congenital heart disease.
- Pulmonary embolism. Part of the blood clot that breaks off in a deep vein is carried by the bloodstream to the lungs. It can block arteries and cause a situation that is extremely life-threatening.
- Blockage of veins by blood clots, resulting in a complete blockage of blood flow in the vein.
Causes of thrombosis and its signs
- If the integrity of the vascular wall is compromised, the development of thrombosis begins. This usually happens as a result of injuries, during pregnancy, when the vessels narrow and become deformed, or if the doctor’s recommendations are not followed after operations.
- When blood stagnation occurs - due to insufficient physical activity or prolonged bed rest. Venous congestion often leads to deep vein thrombosis and varicose veins. To reduce the risk of developing blood clots, it is recommended to use venotonic agents for varicose veins: for example, Normaven® Leg Cream. This product was developed by specialists from the pharmaceutical company VERTEX, has undergone clinical studies and has all the necessary documents and quality certificates confirming its effectiveness and safety. As a result of the testing, it was found that a three-month course of using Normaven® Leg Cream helps to improve the condition of the blood vessels of the lower extremities, due to which cramps disappear, the severity of the venous pattern decreases, swelling and a feeling of heaviness in the legs disappear.
- When the number of platelets and red blood cells in the blood increases, blood clotting parameters change. The cause may be hormonal imbalances, metabolic disorders and oral contraceptives.
- Thrombosis can develop in patients with cancer, as well as with kidney dysfunction.
Factors that increase the risk of thrombosis:
- injuries;
- obesity and excess weight;
Obesity and excess weight are factors in the development of thrombosis
- pregnancy and childbirth;
- smoking;
- infections;
- long-term and frequent trips and air flights;
- age from 40 years;
- taking medications that increase blood clotting;
- surgical intervention on joints and abdominal operations under anesthesia;
- bone fracture;
- sedentary lifestyle.
Diet
People suffering from TF or at risk of developing this disease should eat as little as possible foods containing vitamin K, which stimulates blood clotting. These products include:
- Bananas;
- Cabbage;
- Pork liver;
- Black currant;
- Soy;
- Beans, etc.
You should also be careful about foods that are involved in the formation of blood clots:
- Confectionery and baked goods.
- Fat meat.
- Canned food.
- Sausages.
- Walnuts.
It is recommended to limit the consumption of salt, sugar, sour cream and butter, and include more plant foods in the diet, including herbs, fresh fruits and vegetables, and grains. Consumption of lean meat and seafood is allowed.
People suffering from TF should eat beef liver, which strengthens the walls of blood vessels, as well as buckwheat, melon, oatmeal, cinnamon, ginger, onions, citrus fruits, dairy products, etc. It is best to steam, or boil or stew foods. Fried, salted and smoked foods are excluded. The daily volume of fluid consumed should not be less than 2.5 liters, not counting strong tea, carbonated drinks and coffee.
What increases the risk
There are diseases in which thrombosis occurs more often:
- Antiphospholipid syndrome
- Atherosclerosis
- Coronavirus infection
- Obesity
- Family history of thrombosis
- Arrhythmias
- Acute heart disease
- Pregnancy
- Prolonged sitting or bed rest
- Smoking
- Operation
Each of these diseases or conditions increases the risk of thrombosis. For example, smoking narrows blood vessels and disrupts blood flow, and with obesity, atherosclerotic plaques are more likely to form.
Prevention of thrombophlebitis
If you have questions about how to treat thrombophlebitis and what measures to prevent it, you should contact a competent phlebologist. He will give precise recommendations regarding activities that will reduce the likelihood of developing the disease. People with two or more risk factors should definitely see a specialist. Prevention, carried out in time, will help eliminate the inflammatory process and the formation of blood clots in the veins. Prevention of the disease is also carried out to prevent its complications. Preventive measures include:
- Massage.
- Healthy lifestyle.
- Proper nutrition.
- Choosing the right clothes and shoes.
- Taking care of hygiene.
- Constant physical activity.
- Timely elimination of colds and infections.
Walking, swimming, cycling and dancing will have a positive effect on your health. Hardening procedures will help strengthen the walls of blood vessels.
Causes of thrombophlebitis
The main causes of venous thrombosis:
- inflammatory process (local and/or general),
- slowing down the flow of blood through the venous vessels, leading to venous stagnation (for example, due to varicose veins),
- hereditary or acquired tendency of the blood to form blood clots (coagulopathies or thrombophilic conditions),
- damage to the venous wall (sometimes even minor trauma to the vessel, for example, catheterization of a vein).
What can be done for thrombophlebitis?
For patients with thrombophlebitis of the legs, regular moderate physical activity is recommended, as well as wearing compression stockings during the day on an ongoing basis. Daily walking in comfortable shoes will also help improve the condition of a person suffering from TF. Physical activity is allowed, but the degree of its intensity must be determined together with the attending physician based on the stage of development and type of pathology, as well as the individual characteristics of the patient’s body.
Treatment of thrombosis
The objectives or goals of the treatment are very specifically formulated today:
1. Stop the spread of thrombosis.
2. Prevent pulmonary embolism.
3. Prevent the progression of edema and prevent venous gangrene.
4. Restore the patency of the veins and the function of the valve apparatus in order to further avoid the development of post-thrombophlebitic disease.
5. Prevent recurrence of thrombosis.
Conventionally, modern approaches to the treatment of patients with acute phlebothrombosis in the inferior vena cava can be divided into three main ones:
1. Conservative.
2. Minimally invasive.
3. Surgical aggression.
Conservative therapy
The set of measures of this approach includes:
- early activation using elastic compression,
- anticoagulant,
- nonspecific anti-inflammatory therapy,
- hemorheological therapy,
- intermittent pneumocompression.
With the timely use of the above methods, it is possible to restore the patency of the veins and minimize the manifestations of post-thrombotic disease.
Minimally invasive methods
Today, this is the most common group of methods in clinical use, designed to solve all of the above problems or goals of treating patients with deep phlebothrombosis.
Here it is necessary to distinguish three subgroups of methods:
1. Installation of vena cava filters and partial cavaplication.
2. Regional and systemic thrombolysis.
3. Catheter thrombus extraction and pharmacomechanical thrombectomy.
Installation of vena cava filters and partial cavaplication
At the beginning of the formation of phlebology as a separate scientific specialty, one of the main issues requiring immediate resolution was the issue of preventing pulmonary embolism in phlebothrombosis. After the development in 1959 of the method of external plication of the vena cava with mattress sutures and external plication with clamps, it was possible to determine the further direction of solving the problem of acute deep phlebothrombosis and its complication - pulmonary embolism. Until 1967, the method in combination with conservative therapy remained the only clinical approach to this problem. Despite the fact that the technology of external partial clipping with clamps is associated with the need for traumatic surgical access and is practically impossible in seriously ill patients, this approach has been used and improved in limited situations to this day (for example, using endovideoscopic techniques, plication from a mini-approach).
The Mobin-Addin intraluminal vena cava filter, created and applied clinically, which required studying methods for delivering the device to the object, was the first experience of intraluminal catheter intervention and, in fact, served as the beginning of the development of a new branch of angiology - interventional radiology. Further development of this direction was carried out mainly along the path of improving the design of vena cava filters and studying their effect on hemodynamics and the clinical course of the main process.
Currently, temporary vena cava filters are preferred. The temporary vena cava filter is removed no later than the third week.
In the vast majority of cases, installation of a vena cava filter is not required at all.
Why is it not advisable to install a permanent vena cava filter?
You should always remember that a permanent vena cava filter means a lifelong use of anticoagulant drugs and a lifelong risk of filter thrombosis (a foreign body in the lumen of the vein is often complicated by thrombosis).
It has been repeatedly noted that as a result of the installation of vena cava filters, pulmonary embolism may occur in the immediate period with a frequency of 1.5-8%, and in a period of up to 3 years, thrombosis of the inferior vena cava occurs with a frequency of 12-25%.
For thrombosis below the inguinal ligament, installation of a vena cava filter is not advisable, since there are other methods for preventing pulmonary embolism.
Regional and systemic thrombolysis, catheter thrombus extraction, rheolytic thrombectomy
Thrombolytic therapy. The method is based on the administration of drugs that activate endogenous fibrinolysis (streptokinase, urokinase, tPA, etc.).
Apparently because the means of influencing the blood clot used in this method can only be effective in relatively fresh areas of the blood clot (up to 3-5 days), so its effectiveness is low. Meanwhile, the use of regional catheter thrombolysis in 44% of cases allowed some authors to preserve valve function and thereby prevent the development of postthrombotic disease.
Catheter thrombus extraction . It should be immediately clarified that this method is applied only to high segments of the inferior vena cava basin, since the technology itself does not allow its application in the infrainguinal position due to the obstacles formed by the valve apparatus of the veins at this and lower lying levels. The method is based on capturing thrombomass from accessible segments of the inferior vena cava and iliac veins into a special container bag and removing them by removing them through a phlebotomy opening.
Pharmaco-mechanical thrombectomy . The newest of all interventional and surgical technologies. So far, there are descriptions of individual cases in the literature. The method is based on the Bernoulli effect, where the speed of a hydrodynamic jet creates areas of negative pressure in the surrounding media. The method has the same scope as catheter thrombectomy.
Surgical interventions for femoropopliteal phlebothrombosis
It is known that the most effective thrombectomy is possible only for blood clots no more than 3-7 days old.
Currently, most authors still adhere to cautious tactics when surgically removing thrombus masses from the femoropopliteal segment, completing the operation by ligation or resection of the ostial segment of the proper femoral vein, assessing the immediate results as good due to the lack of severity of symptoms of chronic venous insufficiency. The calculation with this approach is to switch the main venous flow to the deep vein of the thigh, which should provide a stable main outflow. In some cases, arteriovenous fistulas are used to prevent rethrombosis.
A number of researchers use the tactic of surgical antegrade thrombectomy without subsequent ligation or ligation of the femoral vein itself, in some cases supplemented by plication of the femoral vein itself or without it.
What is prohibited for thrombophlebitis?
If a person develops a disease, he is strictly prohibited from:
- Wear uncomfortable high-heeled shoes.
- Lift heavy objects.
- Engage in sports that involve intense stress on the limbs.
TF of deep veins is a restriction for visiting saunas, drinking bowls and baths. This is due to the fact that high temperatures significantly accelerate blood circulation, which has an extremely negative effect on the course of the disease.
It is strictly forbidden to gain extra pounds, and therefore a person must pay special attention to proper nutrition. Animal fats, which can be replaced with vegetable oils, should be excluded from the diet. The amount of salt consumed should be kept to a minimum in order to eliminate swelling. Quitting alcohol and smoking is mandatory for TF.
Diagnosis of the disease
When visiting a medical facility, the doctor makes a diagnosis and prescribes treatment. Basic diagnostic methods:
- Blood tests for clotting
- Magnetic resonance venography
- Duplex/triplex scanning of the arteries of the lower extremities
- Duplex/triplex scanning of the veins of the lower extremities
- Duplex/triplex scanning of extracranial brachiocephalic arteries
- Duplex/triplex scanning of intracranial brachiocephalic arteries
- Duplex/triplex scanning of arteries and veins of the upper extremities
- Ascending venography using contrast agent
- Radionuclide scanning of thrombus location
- Thromboelastography.
Specialists to contact:
- Phlebologist
- Vascular surgeon
- Cardiologist
- Neurologist, etc.
The difference between thrombophlebitis and varicose veins
TF and varicose veins have similar symptoms. However, their nature is different. In the case of varicose veins, the vessels are dilated and their walls are thinned. The result is impaired blood flow and the formation of nodes. In the case of thrombophlebitis, inflammation of the venous walls and thrombus formation occurs. The thrombus clogs the lumen of the vessel, which leads to disruption of blood flow and swelling of the affected vessel.
The key difference between the diseases lies in the pathological mechanisms underlying each of them. Disruption of the functions of the valvular venous apparatus and excessive expansion of their lumen occurs as a consequence of destructive changes in the vessels formed under the influence of harmful factors. But the pathology occurs only with impaired blood circulation in the venous line and trophism of the soft tissues located around the affected vessel. A complication of varicose veins that cannot be treated is thrombophlebitis.
Symptoms of thrombosis
The clinical manifestations of this pathology vary depending on the location.
Symptoms of venous thrombosis
When a vein is blocked, the outflow of blood is hampered, so the tissues beyond the blockage swell and turn blue. The waste products of cells accumulate, therefore tissue intoxication develops, this is accompanied by pain, impaired sensitivity (the sensation of “crawling goosebumps”). If you do not intervene in time, the tissues begin to die.
Symptoms of venous thrombosis of the lower extremities:
- swelling of the leg, a sharp increase in size, cyanosis;
- cramps of the calf muscles;
- constant pain in the leg, which intensifies when walking;
- increased venous pattern on the thigh.
Cavernous sinus thrombosis:
The dura mater contains channels into which venous blood from the brain drains. Blockage of one of these sinuses, the cavernous sinus, is dangerous because several cranial nerves and the internal carotid artery pass through it. The most common causes of cavernous sinus thrombus formation are inflammatory diseases of the nose, sinuses, facial skin and scalp. Signs:
- headache;
- decreased visual acuity, double vision;
- confusion;
- heat, fever;
- swelling of the eyelids and periocular area;
- pain in the neck when turning or tilting the head;
- impaired facial skin sensitivity.
Among the consequences of such thrombosis: stroke, loss of vision, coma.
Hemorrhoidal thrombosis
Develops against the background of hemorrhoids. Chronic constipation, physical stress, pregnancy and childbirth, and alcohol abuse contribute to it. Signs:
- pain, burning and itching in the anal sphincter area;
- discharge of blood with feces and regardless of the act of defecation;
- prolapse of hemorrhoids.
Retinal vascular thrombosis
The pathology is a typical complication of diabetes mellitus and hypertension, but can also develop for other reasons. Symptoms:
- deterioration of vision, up to complete loss (usually one-sided);
- the appearance of spots, mesh, veils before the eyes.
Symptoms of arterial thrombosis
Blockage of the artery leads to oxygen and energy starvation of tissues, which quickly leads to their death. Arterial forms of the disease are often acute.
Thrombosis of the cerebral arteries
This process leads to necrosis of the area of the brain that the affected artery supplies blood to - ischemic stroke. Signs:
- hemiparesis ー lack of movement in the right or left half of the body (opposite affected area);
- asymmetry of the smile - one corner of the mouth is lowered, does not take part in conversation and smile;
- unclear speech;
- when the patient sticks out his tongue, it deviates to the side.
Thrombosis of the coronary arteries of the heart
Partial blockage of these vessels leads to attacks of angina pain, complete blockage leads to myocardial infarction. Symptoms:
- pressing, burning pain behind the sternum, radiating to the left shoulder blade, arm, shoulder, half of the face and neck;
- dyspnea;
- with angina pectoris, rest and nitroglycerin help, with a heart attack there is no improvement, urgent medical attention is needed.
Pulmonary artery thrombosis
It is a complication of thrombosis of the veins of the lower extremities, endocarditis, myocardial infarction. It develops rapidly and has a high mortality rate. Signs:
- sharp stabbing pain in the chest;
- swelling of the veins of the neck;
- shortness of breath, feeling of lack of air;
- hemoptysis;
- increased heart rate.
Hepatic artery thrombosis
Death (infarction) of liver tissue is a complication of endocarditis, myocardial infarction or liver transplantation and manifests itself as follows:
- severe pain under the right rib;
- nausea, vomiting, bitterness in the mouth;
- yellowness of the skin and whites of the eyes.
Femoral artery thrombosis
This form of pathology is manifested by pain when walking, coldness, and paleness of the limb. The pulse in the popliteal fossa and on the foot is palpable weakly or not detected at all.
How to determine deep vein thrombosis
Considering the high risk of developing complications in the form of pulmonary embolism, pulmonary hypertension and post-thrombotic syndrome, if deep vein thrombosis is suspected, it is necessary to urgently seek qualified medical help. The Yusupov Hospital guarantees all patients timely and high-quality diagnostics using modern expert-class equipment. The clinic’s doctors, having deep knowledge in the field of angiology and phlebology, can easily make the correct diagnosis and select effective treatment tactics.
To make an accurate diagnosis, a combination of several factors is required, namely:
- Clinical assessment of the likelihood of thrombosis. At the moment, the Wells scale is used for this purpose;
- Results of clinical and laboratory tests - determination of the level of D - dimer, diagnosis of the state of the blood coagulation system (coagulogram);
- Data from instrumental research methods: venous Dopplerography, venography, MRI, impedance plethysmography;
- Functional tests.
When objectively examining a patient for the presence of deep vein thrombosis of the lower extremities, based on the localis status and the results of functional tests, a competent phlebologist can determine the presence of a blood clot, even without special diagnostic equipment. Among the most reliable tests used today in phlebology are the following:
- Marching test - the patient is asked to walk for several minutes, tying an elastic bandage around the leg from the toes to the groin area. If after this short walk the patient develops bursting pain in the lower leg and dilated saphenous veins are visualized, then the diagnosis of thrombosis is confirmed;
- Lowenberg's sign - the doctor places a pressure cuff above the knee and pumps pressure into it. Painful sensations appear when the pressure is 80 – 100 mm Hg, which corresponds to a sign of vein blockage;
- Homans test - the patient lies on his back, with his legs bent at the knees. Signs of thrombosis (pallor and sharp pain in the calf area) appear when the foot is flexed;
- Mayo-Pratt test - after a preliminary massage (to empty the superficial veins), I apply a tourniquet to the upper third of the thigh. The patient is asked to walk in this state for 35 to 40 minutes. A feeling of fullness and the appearance of pain indicate thrombosis of the deep veins of the lower extremities;
- Brodie-Troyanov-Trendelenburg test - the patient lies on his back with his leg raised up. Then a rubber band is placed in the middle of the tourniquet and asked to quickly take a vertical position. Rapid filling of the veins below the tourniquet indicates a disruption of the veins;
- Hackenbruch test - the doctor clamps the place where the saphenous vein flows into the femoral vein. Then he asks the patient to cough and the shock he feels under his fingers is created by a reflected wave from the blood clot.
D-dimer is a fibrin breakdown product that is formed as a result of activation of fibrinolysis processes (dissolution of blood clots). Although it is the best biomarker for early diagnosis of thrombosis, the D-dimer assay has a high probability of producing a false-positive result.
Doppler sonography is one of the most reliable methods for diagnosing the presence of a blood clot. During the examination, the doctor receives a complete picture of the movement of blood through the vessels.
Phlebography is the injection of an absolutely harmless contrast agent into a vein, due to which the course of the vessel is clearly visible on X-ray photographs, and a thrombus is described as a round formation nearby in the lumen of the vessel.
Impedance plethysmography - determination of impedance between two electrodes located on the lower leg. An inflated cuff located in the middle third of the calf region obstructs the outflow of venous blood, thereby causing a rapid change in resistance. This method is safe and non-invasive.
Magnetic resonance imaging (MRI) is the most accurate method for diagnosing deep vein thrombosis of the lower extremities. It has high sensitivity and specificity. Its help is resorted to in cases where, for certain reasons, venography is contraindicated.
The Yusupov Hospital has a huge advantage over other Moscow clinics due to the presence of a powerful diagnostic base. Patients note the professionalism of doctors in their work, which affects satisfactory results.