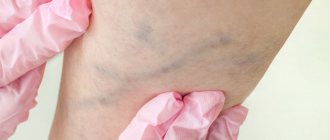
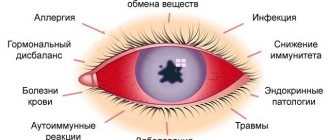
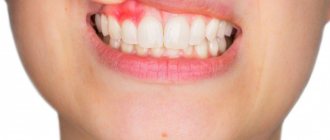
Risk factors (reasons for development)
Psoriasis occurs in approximately 3% of the world's population, regardless of gender. It begins at any age, but most often between 15 and 30 years. There are cases of the disease being detected in infants. The highest prevalence is among representatives of the Caucasian race, less often among the Negroid and Mongoloid races.
The disease is characterized by a wave course with periods of exacerbation and remission. Has an acute onset in most cases. A monomorphic rash of papules merges into larger plaques, which are then covered with white scales.
The etiology and pathogenesis of skin pathology have not been fully studied; both hereditary predisposition and neurogenic nature are assumed. Many patients note that the disease manifests itself and subsequently intensifies during periods of greatest stress. Some researchers believe that the cause of the disease may be an infection, but the virus has not been identified. This theory is contradicted by the fact that the patient’s immediate environment does not get sick, and the presence of psoriasis in the family history increases the likelihood of its diagnosis in descendants.
Etiology and pathogenesis
Among the causes of psoriasis are the following:
- Genetics - the disease is associated with certain human leukocyte antigen (HLA) alleles, the most “strong” of which is HLA-Cw6. Other associated alleles are HLA-B27, HLA-B13, HLA-B17 and HLA-DR7.
- Immunology - The immunological concept of psoriasis is supported by high levels of cutaneous and circulating tumor necrosis factor alpha (TNF-α), as well as the fact that treatment with TNF-α inhibitors often puts patients into remission. In addition, it was noted that after certain immunological events, guttate psoriasis can occur - for example, after streptococcal pharyngitis, cessation of corticosteroid therapy, etc.
- Obesity is an incompletely studied factor. Whether excess weight alone, a genetic predisposition to obesity, or a combination of these factors influences the development of psoriatic plaques is not known. However, it has been noted that with an increase in body weight, the condition of psoriasis worsens, as well as vice versa, with a decrease in weight, the course of the disease improves.
- Stress and the environment - psychological experiences can both provoke the development of psoriasis and aggravate it. Exacerbations of the disease are also caused by injuries, infections (streptococcus, staphylococcus, human immunodeficiency virus), alcohol, and medications (aspirin, beta-blockers). One study documented an increase in the incidence of psoriasis flare-ups in patients with chronic gingivitis. Treatment of gingivitis allowed us to go into remission, but did not affect the disease in the long term, which once again emphasizes the complexity and multifactorial nature of psoriasis.
Interestingly, 2.5% of people with HIV develop progressive psoriasis due to decreased CD4 T cell counts. This does not fit into modern understanding of the disease ( Fig. 1 ), since the leading hypothesis states that T cells are hyperactive in psoriasis , and treatment aimed at reducing their number usually reduces the severity of psoriasis. It is possible that a decrease in the number of CD4 T cells in patients with HIV leads to an increase in the activity of CD8 T cells, which causes the progression of psoriasis.
Rice. 1. General understanding of the etiology and pathogenesis of psoriasis, as well as the development of associated conditions (World Health Organization, WHO)
- The first sector (internal, shaded) is genetics, environmental triggers.
- The second sector is microinflammation, insulin resistance, obesity.
Two internal sectors include the basic predisposing factors and pathogenetic components of psoriasis. The main clinical sign is inflammation ( Inflammation ).
- The third sector is myocardial infarction, atherosclerosis, stroke, metabolic syndrome.
- The fourth sector is depression, anxiety disorders.
The two middle sectors reflect the transition to systemic lesions - from cutaneous psoriasis to psoriatic arthritis ( Psoriasis - Arthritis ) and related problems. Main clinical signs: cardiovascular pathologies ( CVD ), psychiatric complications ( Psychiatry ).
- The fifth sector is patient stigmatization, increased cost and duration of treatment, and lack of satisfaction with therapy.
- The sixth sector (outer, with an arrow) - smoking, alcohol abuse, possible secondary obesity, addiction, compliance (level of adherence to treatment)
The two external sectors reflect the consequences of the disease ( Consequences ) and the patient's quality of life ( Qol ), as well as the burden of psoriasis ( BoD ), i.e. deterioration in a person’s quality of life due to illness.
https://apps.who.int
Manifestations of psoriasis
At the first stage, the disease manifests itself in the form of a single pink papule. It changes, increases in size, grows above the skin, and becomes covered with white scales. More often, psoriasis plaques appear in places of friction and increased pressure on the skin: buttocks, elbows and knees. As the disease progresses, they can be found absolutely anywhere on the skin, including the scalp.
Main clinically diagnosed external signs:
- Stearic stains, i.e. easy separation of flakes by scraping.
- The terminal film remaining after the scale is removed. It looks like a smooth, shiny, even pink surface.
- Pinpoint bleeding, which can be caused by removing the scale.
Psoriasis develops quite slowly; an increase in the number of plaques and their growth can be observed over several months or years. In a small percentage of patients, the disease may manifest itself more intensely. As a rule, this is preceded by severe mental stress or a serious illness requiring massive drug treatment. In this case, the papules are not pale pink, but bright red, with obvious signs of inflammation, swollen, causing itching.
The second stage of psoriasis is characterized by more extensive lesions. At the site of scratching, new papules appear, forming new plaques. As a result of peripheral growth, new growths merge with existing ones. Plaques affect symmetrical limbs and form similar patterns and lines.
At the third stage, growth slows down, changes concern mainly the structure of the rash. The boundaries between healthy and affected skin become clearer. The plaques acquire a bluish tint and begin to actively peel off. In the absence of therapy, they thicken and sometimes form papillomatous nevi (brown) and warty growths (flesh-colored).
There is another stage - regression of the disease, at which time the symptoms fade away. Peeling goes away, the clarity of the border disappears, the skin normalizes and returns to its original state.
What cosmetics to choose for psoriasis
For all forms of psoriasis (both winter and summer), the choice of cosmetics is very important. Conventional cosmetics may contain additives and fragrances that can cause skin irritation. Therefore, it is best to use specialized cosmetics not only during an exacerbation, but also constantly.
La Cree, a series of products for sensitive, rash-prone skin, is designed specifically for such cases. These products (creams, gels, etc.) can be used even on irritated skin due to their safe composition based on natural ingredients. Cosmetics do not contain hormones.
La-Cri cream is ideal for irritation-prone skin. It reduces hypersensitivity, softens inflammation, redness, peeling and itching. Thanks to these properties, it can be used after burns and insect bites. The cream can be used for a long time: it is also suitable for newborns and pregnant women.
The complex effect of the cream is due to the natural plant extracts it contains. For example, licorice and string extract relieves itching, reduces redness and inflammation. Violet and chamomile extracts also soothe the skin and soften breakouts. Regeneration processes in skin cells are restored by panthenol and avocado oil. These same components moisturize and nourish the skin. The cream also prevents infections in the affected areas due to the content of walnut extract, which heals wounds and fights germs.
La-Cri cream is recommended for use for any skin conditions complicated by inflammation and itching, including sunburn, allergies after insect bites, burns from nettles and other plants, and diaper rash in children.
The cream is applied to cleansed skin once or twice a day. For widespread psoriasis, La-Cri cream can be used both once and for a long time.
Classification of psoriasis
The disease has many types, but they are all divided into two main types:
- Non-pustular psoriasis (simple, plaque, erythrodermic).
- Pustular psoriasis (generalized, palmoplantar, annular psoriasis, persistent acrodermatitis, impetigo).
A number of disease researchers identify the following types of psoriasis:
- drug-induced
- reverse type,
- seborrheic;
- Napkin's psoriasis (occurs in infants in the diaper area).
According to ICD-10, plaque psoriasis, inverse psoriasis, guttate psoriasis, pustular psoriasis, nail psoriasis (onychodystrophy), psoriatic arthritis and erythrodermic psoriasis are distinguished. Let's look at common forms in more detail.
Pustular form of psoriasis
It is characterized by the presence of plaques with cortical scales, impregnated with exudate. If damaged, for example, as a result of scratching or self-injury in the folds of the body, the rashes become wet. They cause itching and burning and cause physical discomfort. This type of disease is more often diagnosed in people with excess body weight, hypothyroidism and diabetes.
Seborrheic type
Affects the scalp. Occurs in people with dandruff and oily seborrhea. This makes diagnosis difficult at the initial stage of development. Over time, psoriasis lesions grow. They can spread to the skin of the forehead, to the ears, to the back of the neck.
Psoriasis of the hands, feet and nails
The main rash occurs on the extremities, with only isolated papules on the body. The affected nail plates become deformed, turn yellow, and thicken. They can go away painlessly. A psoriatic border may form around the affected area. There are subungual hemorrhages that look like dark red spots, which then turn black.
Pustular (generalized) form
It has a classic pattern of development, starting with a single vesicle that develops into plaques. The lesions are symmetrical and can affect any part of the body. The severe course of this form of psoriasis is characterized by the appearance of intraepidermal pustules. They can unite, forming “purulent lakes.” The pustules do not open on their own, since they are externally protected by a dense brown crust.
Arthropathic form
The most severe form of psoriasis, in which changes first affect small joints, and then large ones, including the spine. This is expressed by pain symptoms and their deformation. Joint fusion and loss of mobility are likely. Against the background of this form of psoriasis, other pathologies arise: ankylosis, osteoporosis, which leads to disability.
conclusions
Pustular psoriasis is a severe form of the disease that requires examination by a doctor. Symptoms:
- red, inflamed spots with blisters (pustules);
- sometimes their localization is only on the palms and feet, sometimes on other parts of the body;
- fever, high temperature, malaise.
Pustular psoriasis can occur due to infections, improper external treatment, and withdrawal of corticosteroid medications. Treatment is carried out only by a doctor. For internal therapy use:
- antipyretic drugs;
- corticosteroids;
- vitamin A analogues and others.
Effective in external therapy:
- zinc ointment with hydrocortisone;
- corticosteroid creams;
- ointments with analogues of vitamins A, D3.
In case of a stable course of the disease, PUVA therapy, Re-PUVA therapy, and ultraviolet irradiation at 311 nm are used. Sanatorium-resort treatment (Sochi, Pyatigorsk) also gives results
Diagnostic methods
The diagnosis and treatment of psoriasis is carried out by dermatologists. Initially, an external examination of the affected areas is carried out, and an anamnesis is collected. Sometimes the disease is similar to other diseases, especially in the first stage. If the hands and nails are affected, it is important to exclude the presence of fungal infections. The seborrheic type also requires differential diagnosis. Seborrheic eczema, pityriasis rosea and papular syphilis should also be excluded.
In case of active disease and large lesions, visual analysis of scrapings is used. In the process of scraping, peeling intensifies. In place of the removed scale, a smooth, thin film is visible. When mechanically applied, it moves away, revealing a moistened surface with droplets of blood.
In most cases, diagnosing psoriasis is not difficult; it does not even require testing; it is enough to examine the skin. However, the doctor must rule out an error in the diagnosis, determine the presence of concomitant diseases and other pathologies occurring against the background of psoriasis. For this purpose, the following diagnostic measures may be prescribed:
- Blood test to detect elevated levels of rheumatoid factor titers, ESR, proteins, leukocytosis, disorders characteristic of endocrine and biochemical pathologies.
- A skin biopsy is performed to confirm psoriasis, clarify its classification and exclude other skin diseases. The nature of the thickening of skin epidermal cells, the presence of Rete accumulation, immunocompetent and other cells are checked.
Laboratory tests are also important when prescribing therapy, to monitor the effectiveness of treatment, and to identify the causes and exacerbation of psoriasis.
How is treatment carried out at the Paramita Oriental Medicine Clinic?
But the first step on the path to getting rid of psoriatic plaques is a preliminary appointment with a specialist. At this appointment, the doctor will determine the nature of the disease, its stage of development, the degree of damage to the skin, and the possible causes of this disease in a particular patient.
Based on the data obtained during the survey - and, if necessary, a laboratory examination is also prescribed - the doctor determines the necessary treatment and prescribes a course of complex therapy sessions.
The cost of preliminary admission is 500 rubles.
Types of analyzes
The main tests performed for psoriasis include:
- Skin biopsy, a piece of skin is examined to differentiate bacterial, fungal infections, and cancer.
- Complete blood count to detect leukocytosis and anemia.
- Erythrocyte sedimentation rate to determine the type of psoriasis. With pustulosis and erythroderma, the indicator remains normal.
- Uric acid test to rule out gout.
- An HIV antibody test is performed because sudden onset of psoriasis can be caused by HIV infection.
- Skin pH testing helps evaluate the effectiveness of the therapy.
If psoriasis affects the joints (arthropathic form), a rheumatoid factor test is performed. It allows you to differentiate rheumatoid arthritis, in which the protein level is increased. Contrast arthrography and pneumoarthrography also help to assess the degree of joint damage.
How to live with psoriasis
If you have psoriatic skin rashes, then from now on you need to change your lifestyle. Even after effective treatment and the disappearance of the symptoms of the disease, it is important not to forget about preventive measures, maintain the correct daily routine, and avoid stress and overwork.
To relieve accumulated tension, it is advisable to engage in sports. Almost any sport will do. Only be careful when swimming in a pool, as the chlorine in the water can cause further irritation to the skin.
Watch your diet, try to get enough sleep, get rid of bad habits. Smoking and alcohol can trigger a relapse of the disease. Also be careful when choosing cosmetics. Ideally, it is best to switch to safe products designed specifically for sensitive skin. In addition, do not forget about vitamin complexes.
If you follow preventative measures, the likelihood of the rash returning will be minimized, and your quality of life will significantly improve.
Be healthy!
Treatment of psoriasis
The basis of treatment for psoriasis is anti-T-cell and anti-cytokine therapy, aimed at reducing inflammation and blocking the proliferation (uncontrolled division) of skin keratinocytes. For exacerbations in winter, a course of cholecalciferol (liquid-soluble vitamin D3) is prescribed. The following medications may be prescribed. To relieve itching, burning, and eliminate skin lesions, the use of anti-inflammatory ointments, gels, and shampoos is recommended. For mild psoriasis, ointments with corticosteroids are prescribed as a course of treatment under the supervision of a physician, salicylic ointment, with naphthalan, mercury. Baths with a decoction of chamomile and/or sage are recommended. Patients undergo ultraviolet therapy and sea water treatment.
Stages of therapy
When treating mild forms of psoriasis, dermatologists try to avoid medications, allowing the body to cope with pathological processes on its own. Usually, local remedies are used first: creams and ointments. If the desired effect is not observed, and the situation continues to worsen, instrumental medicine is used. They conduct courses of UV therapy, wave therapy, and photochemotherapy. Only after the lack of results of this treatment, drugs are prescribed.
Patients with psoriasis are prohibited from drinking alcoholic beverages. A diet with limited consumption of table salt, fats, and carbohydrates is recommended. Taking herbal medicines should be under the strict supervision of the attending physician.
All patients are recommended to visit a psychologist. Often the disease worsens during periods of stress, which means the cause must be removed. Secondly, unaesthetic plaques on different parts of the body, by the fact of their existence, create stress and depression. According to studies, more than half of patients reduce social communication and experience a feeling of awkwardness and shame. Alternative methods of treating psoriasis include the prescription of antidepressants and other psychotropic drugs, diet therapy, hydrotherapy, including the use of fish that eat plaques.
Today, the prognosis for treatment of psoriasis is considered conditionally unfavorable.
The course of the disease is chronic, sluggish, and progressive. The techniques developed by modern medicine can only alleviate the condition, but not cure the disease. At the same time, refusal of medical care can lead to disability over time. Prevention of psoriasis
Based on the fact that psoriasis is considered a multifactorial disease with a share of immunopathological, genetic, endocrine, metabolic and, possibly, infectious components, there are no uniform rules for prevention.
People at risk should pay special attention to their health:
- those who have relatives suffering from psoriasis;
- those who frequently and constantly injure the skin;
- has chronic infections;
- diseases of the nervous system;
- endocrine disorders.
Increased nervousness, stress, alcohol abuse, frequent hypothermia and sunburn increases the likelihood of pathology. Unfortunately, it is impossible to completely protect yourself from destructive manifestations.
Biological drugs created using genetic engineering methods are monoclonal antibodies used for therapeutic purposes. In domestic medical practice, the following biological drugs are approved for medical use for the treatment of psoriasis: infliximab, adalimumab, ustekinumab, etanercept.
1. Infliximab
Infliximab is a selective TNF-a antagonist, which is a chimeric monoclonal IgG antibody that consists of 75% human and 25% mouse protein. Infliximab is indicated for the treatment of adult patients with psoriasis with severe and moderate forms of the disease in the absence of clinical effect from the use of other systemic therapies (including cyclosporine, acitretin, methotrexate and PUVA therapy) or in cases of intolerance or contraindications to their use, as well as for the treatment of active progressive psoriatic arthritis.
Doses and regimens
The drug is administered intravenously by drip for at least 2 hours at a rate of no more than 2 ml/min. under the supervision of medical personnel. For the treatment of psoriasis and psoriatic arthritis, the initial dose of infliximab is 5 mg per kg of patient weight. After the first administration, the drug is administered in the same dose after 2, then 6 weeks. and then every 8 weeks. If there is no effect within 14 weeks. (after four intravenous infusions) it is not recommended to continue treatment. During the intravenous infusion and for at least 1-2 hours after its completion, the patient must be under the supervision of a physician. During intravenous infusion of the drug, it is necessary to measure blood pressure, pulse, and respiratory rate and body temperature every 30 minutes.
Adverse reactions/safety
In clinical studies, adverse reactions were observed in approximately 60% of patients receiving infliximab and 40% of patients receiving placebo.
- Infusion reactions occur during infusions or within 1-2 hours after it. These include swelling of the pharynx/larynx, bronchospasm, chills, headache, hot flashes, nausea, shortness of breath. In clinical trials, the incidence of infusion reactions when using infliximab was about 20%, in the comparison group (placebo) - about 10%. Approximately 3% of patients were forced to discontinue treatment due to the development of infusion reactions, which were reversible in all patients (with or without drug therapy).
- Delayed hypersensitivity reactions in the form of arthralgia, myalgia, fever and rash develop in 1% of patients with psoriasis at the beginning of treatment.
- In clinical trials, when infliximab treatment was repeated 2-4 years after the previous course of therapy, patients experienced adverse reactions (myalgia, arthralgia accompanied by fever and/or rash, itching, swelling of the face, lips or hands, dysphagia, urticaria, pain sore throat and/or headache), which developed 3-12 days after re-infusion.
- Infectious complications are the most common serious side effects. They were associated with approximately 50% of all recorded deaths. There have been cases of tuberculosis, including miliary tuberculosis with extrapulmonary localization, in some cases with a fatal outcome.
- Malignant neoplasms and lymphoproliferative diseases. There have been cases of emergence or recurrence of malignant neoplasms. The incidence of lymphoma in patients treated with infliximab was higher than the expected incidence of this disease in the general population. The incidence of other forms of malignant neoplasms in patients treated with infliximab did not exceed the reported incidence in the general population.
- Cardiovascular failure. Cases of progression of cardiovascular failure during the use of infliximab have been described. There are rare reports of newly diagnosed cardiovascular failure, including in patients who had no previous diseases of the cardiovascular system.
- Changes in the liver and biliary tract. There are very rare reports of the appearance of jaundice and non-infectious hepatitis, in some cases having signs of autoimmune hepatitis, the development of liver failure, leading to the need for a liver transplant or fatal outcome. A cause-and-effect relationship between the occurrence of these adverse reactions and treatment with infliximab has not been established. There have been cases of exacerbation of hepatitis B in patients who were chronic virus carriers (who had a positive reaction to HBsAg).
- When treated with infliximab, a mild to moderate increase in aminotransferase activity may be observed without the development of significant liver damage. In most cases, the increase in aminotransferase levels is transient and asymptomatic. A decrease or return to the initial level of these indicators occurs regardless of whether treatment with infliximab is continued or stopped or concomitant therapy is changed. An increase in alanine aminotransferase activity to a level equal to or greater than 5 times the upper limit of normal was observed in 1% of patients.
- When using infliximab, isolated cases of the development of demyelinating diseases of the central nervous system, optic neuritis, and epileptic seizures have been described.
- In some patients, antinuclear antibodies appeared in the blood serum during treatment with infliximab. Cases of reversible lupus-like syndrome have been described.
Pregnancy/lactation
Infliximab is not recommended for use during pregnancy. During treatment with the drug and for 6 months. after its completion, reliable methods of contraception should be used. Breastfeeding should be discontinued when infliximab is prescribed. Breastfeeding is allowed no earlier than after 6 months. after the end of therapy.
Prevention and treatment of adverse reactions
For early detection of an acute infusion reaction, the patient should be carefully observed during and for at least 1-2 hours after the drug infusion. If an acute infusion reaction occurs, the drug should be discontinued. When conducting infliximab infusions, it is necessary to have appropriate equipment and medications (adrenaline, glucocorticosteroids for parenteral administration, antihistamines, equipment for artificial ventilation). To prevent mild and transient infusion reactions, the patient may be prescribed antihistamines before starting the infusion.
Contraindications/restrictions
- Hypersensitivity reactions to infliximab, other murine proteins, as well as to any of the inactive components of the drug.
- Severe infectious process, for example, sepsis, abscess, tuberculosis or other opportunistic infection.
- Heart failure - severe or moderate.
- Pregnancy and breastfeeding.
- Age less than 18 years.
Interaction
The interaction of infliximab with other drugs has not been studied. Concomitant use with methotrexate in patients reduces the formation of antibodies to infliximab and increases its concentration in plasma.
Overdose
A single administration of infliximab in doses up to 20 mg/kg did not cause direct toxic effects. In case of overdose, observation and immediate relief of symptoms are necessary.
special instructions
- Infliximab, when administered, can cause the development of acute allergic reactions (immediate type) and delayed allergic reactions. Acute infusion reactions may develop immediately or within several hours after administration. A patient receiving infliximab should be monitored during and for at least 1-2 hours after the drug infusion.
- Some patients may develop antibodies to infliximab, which is associated with a more frequent development of infusion reactions. In patients suffering from Crohn's disease, there has been a correlation between the formation of antibodies and a decrease in the duration of the effect of treatment. Patients who stop taking immunosuppressive drugs before or during treatment with infliximab are more at risk of developing these antibodies. If severe reactions develop, symptomatic therapy should be carried out, and further use of the drug should be excluded.
- As the interval between infusions increases, the likelihood of the formation of antibodies to infliximab increases. When re-prescribing infliximab after a long break in treatment, it is necessary to be wary of the appearance of a delayed-type hypersensitivity reaction in the patient.
- When prescribing infliximab to patients with a history of indications of malignant neoplasms, or when deciding whether to continue treatment with infliximab in patients with newly diagnosed neoplasms, special caution should be exercised.
- Before starting treatment with infliximab, the patient should be carefully examined to identify both active and latent tuberculosis. The examination should include:
- careful collection of anamnesis (presence of tuberculosis in the past and/or contact with tuberculosis patients);
- X-ray examination of the chest in two projections;
- conducting a tuberculin test;
- consultation with a phthisiatrician.
- If a tuberculous process is suspected, the use of infliximab should be discontinued until diagnosis is made and, if necessary, appropriate therapy should be administered.
- The patient should be informed that he needs to consult a doctor if the following symptoms appear during treatment with infliximab or after its completion: cough, weight loss, low-grade body temperature.
- During treatment and after its completion, the patient should be closely monitored for signs of possible infection. Since elimination of infliximab occurs within 6 months, the patient should be constantly under medical supervision during this period. Treatment with infliximab should be discontinued if the patient develops a severe infection, including tuberculosis, sepsis or pneumonia.
- The use of live vaccines during treatment with infliximab is not recommended.
- In rare cases, an autoimmune process may develop in genetically predisposed patients. In the event of persistent rash, fever, joint pain, fatigue, or the presence of DNA antibodies in the blood, treatment with infliximab should be discontinued.
- The benefits and risks of infliximab should be carefully weighed in patients with pre-existing or new-onset CNS demyelinating disease.
- Patients with moderate circulatory insufficiency should be carefully monitored. If symptoms of circulatory failure increase, infliximab should be discontinued.
- Patients with signs of liver dysfunction should be evaluated for liver disease. If jaundice occurs or alanine aminotransferase activity increases to levels greater than 5 times the upper normal value, infliximab should be discontinued and a thorough evaluation should be performed.
- Hepatitis B virus carriers should be examined before treatment with infliximab and continuously monitored during treatment in order to timely detect a possible exacerbation of the disease.
- The effectiveness and safety of treatment with infliximab in children and adolescents under the age of 18 years, inclusive, suffering from psoriatic arthritis and psoriasis have not been studied. Until convincing data are obtained, the drug should not be used in these age groups.
- There have been no specific studies on the use of infliximab in elderly people, as well as in people with liver and kidney diseases. There is limited experience indicating the safety of treatment with infliximab in patients undergoing arthroplasty.
Monitoring laboratory parameters during treatment with infliximab
| Infusion weeks | ||||
| Before | 2nd week | 6th week | Every 8 weeks | |
| General blood test1 | X | X | X | X |
| General urine analysis | X | X | X | X |
| ALT,AST | X | X | X | X |
| Pregnancy test | X | |||
Note. 1 Hemoglobin, hematocrit index, erythrocytes, leukocytes, leukocyte formula, platelets.
2. Adalimumab
The selective immunosuppressive drug adalimumab is a completely identical human monoclonal antibody that blocks the activity of TNF-a, a pro-inflammatory cytokine that plays a key role in the pathogenesis of psoriasis. Doses and regimen. For chronic plaque psoriasis, the initial dose for adult patients is 80 mg. Maintenance dose - 40 mg once every 2 weeks, starting a week after the initial dose. The drug is administered subcutaneously into the thigh or abdomen.
Overdose.
The maximum tolerated dose of adalimumab in humans has not been established. Repeated use of adalimumab in doses up to 10 mg/kg was not accompanied by toxic effects requiring dose reduction. In case of overdose, it is necessary to monitor adverse reactions and immediately begin adequate symptomatic treatment.
Drug interactions
In patients with rheumatoid arthritis receiving methotrexate, there is no need for dose adjustment of adalimumab or methotrexate. However, methotrexate with single and repeated use reduces the clearance of adalimumab by 29% and 44%, respectively. The interaction of adalimumab with other drugs other than methotrexate has not been studied in pharmacokinetic studies. In clinical studies, there were no signs of interaction of adalimumab with other basic drugs (sulfasalazine, hydrochloroquine, leflunomide and parenteral gold preparations), corticosteroids, salicylates, NSAIDs and analgesics.
Pregnancy and lactation.
Adalimumab is contraindicated during pregnancy and breastfeeding. Adequate and strictly controlled studies of the drug in pregnant women have not been conducted. Women of reproductive age should avoid conceiving while being treated with the drug. Given the risk of serious side effects in the newborn, it is advisable to stop breastfeeding or discontinue the drug, taking into account its importance for the mother.
Side effects
- According to clinical studies, approximately 15% of patients can be expected to develop injection site reactions, which are one of the most common side effects with adalimumab in controlled clinical trials.
- Infections: very often - respiratory tract infections (including upper and lower respiratory tract infections, pneumonia, sinusitis, pharyngitis, nasopharyngitis and herpes viral pneumonia); often - generalized infections (including sepsis, candidiasis and influenza), gastrointestinal infections (including viral gastroenteritis), skin and soft tissue infections (including paronychia, cellulitis, impetigo, necrotizing fasciitis and herpes zoster), ear infections, oral infections (including herpes simplex, oral herpes and dental lesions), genital infections (including vulvovaginal mycotic infection), urinary tract infections (including pyelonephritis); uncommon - opportunistic infections and tuberculosis (including coccidioidomycosis, histoplasmosis and complex of infections caused by Mycobacterium avium), neurological infections (including viral meningitis), eye infections, bacterial infections, joint infections.
- Neoplasms: often - benign neoplasms, skin cancer, except melanoma (including basal cell carcinoma and squamous cell carcinoma); uncommon - lymphoma, parenchymal neoplasms, neoplasms of the mammary gland, lungs and thyroid gland, melanoma.
- From the blood and lymphatic system: very often - leukopenia (including neutropenia and agranulocytosis), anemia; often - thrombocytopenia, leukocytosis; uncommon - idiopathic thrombocytopenic purpura; rarely - pancytopenia.
- From the immune system: often - hypersensitivity reactions, seasonal allergies.
- Metabolism: very often - increased lipid levels; often - hypokalemia, increased uric acid levels, pathological changes in sodium content, hypocalcemia, hyperglycemia, hypophosphatemia, increased potassium levels in the blood; infrequently - dehydration.
- From the nervous system: very often - headache; often - paresthesia (including hypesthesia), migraine, sciatic neuralgia, mood changes (including depression), irritability, insomnia, dizziness; infrequently - tremor; rarely - multiple sclerosis.
- From the senses: often - conjunctivitis, visual impairment; infrequently - blepharitis, eyelid edema, diplopia, deafness, ringing in the ears.
- From the cardiovascular system: often - arterial hypertension, hot flashes, hematomas, tachycardia; uncommon - arrhythmia, congestive heart failure; rarely - cardiac arrest, arterial occlusion, thrombophlebitis, aortic aneurysm.
- From the respiratory system: often - cough, asthma, dyspnea; infrequently - chronic obstructive pulmonary disease, interstitial lung diseases.
- From the digestive system: very often - nausea, vomiting, abdominal pain, increased activity of liver enzymes; often - dyspepsia, gastroesophageal reflux, dry mouth (sicca syndrome), gastrointestinal bleeding; uncommon - pancreatitis, dysphagia, facial edema, cholecystitis, cholestasis, increased bilirubin levels, hepatic steatosis.
- Dermatological reactions: very often - rash (including exfoliative); often - itching, urticaria, hemorrhages (including purpura), dermatitis and eczema, brittle nails, hyperhidrosis; Uncommon: night sweats, scars.
- From the musculoskeletal system: very often - musculoskeletal pain; often - muscle spasms; uncommon - rhabdomyolysis; rarely - systemic lupus erythematosus.
- From the urinary system: often - hematuria, renal failure; infrequently - nocturia.
- From the reproductive system: infrequently - nocturia, erectile dysfunction.
- From laboratory indicators: often - violations of indicators
- blood clotting (including increased aPTT), positive tests for autoantibodies (including antibodies to the double helix of DNA), increased LDH levels.
- Local reactions: very often - reactions at the injection site (including erythema).
- Other: often - chest pain, swelling; infrequently - inflammation, deterioration of wound healing.
special instructions
.
Adalimumab has a number of important features. In particular, the drug has no risk of infusion reactions, since adalimumab is administered subcutaneously. The frequency of formation of antibodies to adalimumab is only 1.9-8.4%, which undoubtedly has a beneficial effect on both the safety profile of long-term use of the drug and has a positive effect on the level and duration of clinical response to treatment.
Long-term follow-up of psoriasis patients treated with open-label adalimumab over 3 years in the large REVEAL study is available. The effectiveness and safety of continuous therapy with adalimumab in patients with moderate to severe psoriasis for more than three years was assessed. The studies demonstrated that in patients with clinical responses to treatment PASI 75, PASI 90 and PASI 100, reflecting a decrease in the extent and severity of the skin process by 75%, 90%, 100%, respectively, the effectiveness of adalimumab was maintained for three years. Thus, after 160 weeks of continuous treatment with this biological agent, the percentage of patients with PASI 75 remained at 76%; PASI 90 - respectively 50%; PASI 100 - 31%. The data obtained suggest that the majority of patients with psoriasis who received adalimumab responded well to treatment carried out for more than 3 years. More than half of the observed individuals after 160 weeks of treatment with adalimumab had only minimal manifestations of psoriasis on the skin, and in one third of the patients the psoriatic process resolved completely. The most stable response to long-term treatment with adalimumab was found in patients with an improvement in PASI 100. The study made it possible to significantly clarify the data on a possible decrease in the effectiveness of the biological agent with long-term use. It was found that it is extremely important to assess response early in treatment with adalimumab. A good initial response rate with adalimumab (PASI 75 or more at weeks 16 and 33) is, in fact, a predictor of favorable long-term treatment outcomes over a follow-up period of 3 years or more. Finally, the study demonstrated the high safety of long-term use of adalimumab. It is important that among all study participants (n=1159), only 2 cases of tuberculosis were registered. Not a single case of lymphoma, lupus-like syndrome, or demyelinating disease was identified.
According to an analysis of the safety of adalimumab in psoriasis, where the assessment was based on data from 13 clinical studies, and the duration of treatment with the drug was up to 5 years, the frequency (expressed as the number of events per 100 PL) of serious AEs, severe infections, malignant neoplasms does not increase or even decreases as increasing the duration of treatment.
3. Ustekinumab
Ustekinumab is a fully human IgG1k monoclonal antibody that has high affinity and specificity for the p40 subunit of human interleukins (IL) IL-12 and IL-23. Ustekinumab is indicated for the treatment of patients over 18 years of age with moderate to severe plaque psoriasis, as well as patients with active psoriatic arthritis as monotherapy or in combination with methotrexate.
Directions for use and doses
Ustekinumab is intended for subcutaneous injection. The recommended dose is 45 mg. The second injection is given 4 weeks after the first application, then every 12 weeks. In patients weighing more than 100 kg, the drug is recommended to be used at a dose of 90 mg. For patients in whom the clinical effectiveness of the drug when used every 12 weeks is not sufficiently expressed, the dose of the drug should be increased to 90 mg every 12 weeks. If this dosing regimen is not effective, a dose of 90 mg should be administered every 8 weeks. Resumption of therapy according to the proposed regimen - a second injection 4 weeks after the first use, and then every 12 weeks - was as effective as the first therapy .
Side effects
The following side effects were observed in clinical studies of ustekinumab:
- infections (odontogenic infections, upper respiratory tract infections, nasopharyngitis, inflammation of subcutaneous fat, herpes zoster, viral infections of the upper respiratory tract);
- mental disorders (depression);
- from the central nervous system (dizziness, headache);
- from the respiratory system (pain in the throat and larynx, nasal congestion);
- from the gastrointestinal tract (diarrhea, vomiting);
- from the skin and subcutaneous tissues (itching);
- from the musculoskeletal system (back pain, myalgia, arthralgia);
- general disorders and reactions at the injection site (fatigue, erythema at the injection site, pain at the injection site, reactions at the injection site, including hemorrhage, hematoma, induration, swelling and itching);
- malignant neoplasms (non-melanoma skin cancer, malignant neoplasms of the prostate, intestines, mammary glands and melanoma in situ);
- hypersensitivity reactions (rash, urticaria).
Immunogenicity: Approximately 6% of patients receiving ustekinumab developed antibodies to the drug, which usually had a low titer. There was no clear correlation between the formation of antibodies and the presence of reactions with the injection. Most patients who had antibodies to ustekinumab also had antibodies that neutralized them. In the presence of antibodies to ustekinumab, patients often had lower efficacy of the drug, although the presence of antibodies does not exclude the achievement of a clinical effect.
In post-registration use of ustekinumab, adverse events from the immune system were identified: hypersensitivity reactions (including rash and urticaria), serious hypersensitivity reactions (including anaphylaxis and angioedema); from the skin and subcutaneous tissues: plaque psoriasis.
Pregnancy and lactation
It is not recommended to use the drug during pregnancy; effective methods of contraception should be used during and 15 weeks after treatment with the drug.
A decision should be made to stop breastfeeding while taking the drug or to discontinue ustekinumab therapy.
Contraindications
- Clinically significant hypersensitivity to ustekinumab or any excipient of the drug;
- Children's age (up to 12 years);
- Pregnancy and lactation;
- Serious infectious diseases in the acute phase, including tuberculosis;
- Malignant neoplasms.
Carefully
- Chronic or recurrent parasitic and infectious diseases of a viral, fungal or bacterial nature.
- History of malignant neoplasms.
- Elderly age.
Overdose
During clinical studies, patients were given single intravenous doses of up to 6 mg/kg without the development of dose-limiting toxicity. In case of overdose, it is recommended to monitor the patient's condition for signs and symptoms of side effects and, if they develop, appropriate symptomatic therapy should be started immediately.
special instructions
- Ustekinumab is a selective immunosuppressant and may increase the risk of developing infections and reactivation of latent infections. In clinical studies, serious bacterial, fungal and viral infections were observed in patients using ustekinumab. Ustekinumab should not be used in patients with clinically significant, active infections. Caution should be exercised when using the drug in patients with chronic infections or a history of recurrent infections.
- Before starting to use the drug, the patient should be tested for the presence of tuberculosis. Ustekinumab should not be used in patients with active tuberculosis. If you have latent or active tuberculosis (including a history of tuberculosis), treatment should be started before using ustekinumab. Treatment of tuberculosis should also be started in patients in whom the sufficient effect of previous treatment is unconfirmed. During and after treatment with ustekinumab, patients should be closely monitored for signs and symptoms of active tuberculosis.
- Patients should be warned to seek medical attention if signs and symptoms suggestive of infection appear. If a serious infection develops, the use of ustekinumab should be discontinued and the patient should be under the supervision of medical personnel. Ustekinumab should not be used until treatment for the infection has been completed.
- Immunosuppressants may increase the risk of developing malignancies. In some patients receiving ustekinumab in clinical trials, the occurrence of malignant neoplasms (cutaneous and non-cutaneous forms) was observed. The use of ustekinumab has not been studied in patients with a history of malignancy. Caution should be exercised when prescribing the drug to patients with a history of malignancy, as well as when considering continued treatment with ustekinumab in patients diagnosed with malignancy. All patients over the age of 60 years, as well as those who have previously received long-term therapy with immunosuppressants or UV radiation, should be screened for the presence of non-melanoma skin cancer.
- Serious hypersensitivity reactions, including angioedema and anaphylaxis, have been reported during post-marketing use of ustekinumab. If anaphylactic or other serious hypersensitivity reactions occur, ustekinumab should be discontinued immediately and appropriate treatment should be instituted.
- The patient should not be vaccinated with live vaccines during the period of treatment with ustekinumab, as well as in the period 15 weeks before vaccination (after taking the last dose of the drug) and 2 weeks after vaccination. Caution should be exercised when using live vaccines to immunize family members of a patient receiving ustekinumab, since there is a risk of viral or bacterial release and transmission of infection from these individuals to patients. Long-term treatment with ustekinumab does not suppress the humoral immune response to vaccines containing pneumococcal polysaccharide and tetanus vaccine. Vaccines containing inactivated microorganisms can be used with ustekinumab, but the induced immune response may not be sufficient to prevent disease.
- Concomitant immunosuppressive therapy: The safety and effectiveness of ustekinumab in combination with immunosuppressive drugs and phototherapy have not been studied in patients with psoriasis. In studies in patients with psoriatic arthritis, coadministration with methotrexate did not affect the safety and efficacy of ustekinumab. Caution should be exercised when considering the possibility of simultaneous
- the use of other immunosuppressants and ustekinumab, as well as when switching from therapy with another antipsoriasis biological drug to ustekinumab therapy.
- Use in elderly patients (over 65 years): Of the 4031 patients treated with ustekinumab, 248 were patients over 65 years of age (183 patients with psoriasis and 65 with psoriatic arthritis). In clinical studies, there was no effect of age on clearance or volume of distribution of the drug. Although studies of the drug showed no differences in the safety and effectiveness of the drug in elderly patients over 65 years of age compared with younger patients, the number of elderly patients is insufficient to make a definitive conclusion about the effect of age (or lack thereof) on clinical effectiveness.
Use in children: The safety and effectiveness of ustekinumab in children has not been studied. The drug has not been studied in patients with renal or hepatic impairment.
Special instructions.
Currently, there is data on the effectiveness and safety of continuous therapy with ustekinumab for 5 years in patients with moderate to severe psoriasis. Multicenter, double-blind, randomized, placebo-controlled studies have shown that the effectiveness of ustekinumab remains high with continuous use of the drug for 5 years, and the most common adverse events are upper respiratory tract infections.
Advantages of taking tests in the laboratory of JSC "SZDCM"
- Easy registration and no queues.
- Anonymity and confidentiality of data.
- Accurate diagnostics thanks to the latest equipment.
- Quick availability of results.
- Tactful, qualified staff.
Laboratory terminals operate in St. Petersburg and the Leningrad region, Pskov, Veliky Novgorod and Kaliningrad. You can get tested at any of them, regardless of your place of registration and residence. The laboratories have a single database, which means you can get the result in any department, in a way convenient for you.
Advantages of treatment at the Paramita clinic
Do you have bright rashes on your elbows and knees that are very itchy and flaky? Have you tried all the remedies, but the lesions on the skin are only increasing? Alas, you cannot get rid of psoriatic plaques simply with medications; an integrated approach from experienced specialists in oriental medicine is required.
By contacting the Paramita clinic, you will have the opportunity not only to stop the development of the disease, but also to nullify the appearance of psoriatic plaques on your skin.
In addition to treating the underlying disease, the techniques and methods of oriental medicine used will restore your overall immunity, improve metabolic processes in your body and relieve many other problems.
Sign up for a free initial appointment
Tsaraat and leprosy
Psoriasis has been known to people for a long time: it was difficult not to notice the disease with such striking manifestations as large plaques on the skin, constant itching and flaking. The first descriptions of a skin disease similar to psoriasis can be found in the Old Testament in the Book of Leviticus: there it is called tzaraat. The book of Leviticus is a set of rules by which the Jewish people should live. The rules included in the Old Testament also contain descriptions of diseases that kohanim (priests) must be able to recognize. A member of the community suffering from tsaraat, despite the fact that his skin was covered with strange white spots, was not ordered to be expelled from the settlement - apparently, it was believed that the disease was not contagious. It is unlikely that the priests of that time understood dermatology in the same way as modern doctors, so the name tsaraat most likely denoted not only psoriasis, but also a number of other skin diseases.
The difficulty in finding descriptions of psoriasis in the past is due to the fact that in medical writings it was often called leprosy. The ancient Roman physician Aulus Cornelius Celsus further confused the situation. He described psoriasis in De Re Medica, calling it impetigo, which means “scabs” in Latin. The same term was used to denote lichen in medical books of that time. In the 16th century, Hieronymus Mercurialis tried his best: with his light hand, psoriasis was combined in clinical descriptions with the same leprosy and some other skin diseases.
The classic description of the disease, made in 1809, belongs to the outstanding English physician Robert Willan (Fig. 3a). The very name of the disease “psoriasis” comes from the ancient Greek word ψωριασις (“psoriasis”), which literally translates as “itchy condition.” This term was first used by the Austrian dermatologist Ferdinand Hebra in 1841 (Fig. 3b). The name is absolutely fair, because itching is one of the symptoms of psoriasis, and it is often what worries patients the most. The merit of Ferdinand Gebra is also that he finally separated non-contagious psoriasis from contagious and fatal leprosy.
After a clear description of the disease, dermatologists from different countries began to actively study it. Heinrich Koebner in 1872 established that skin damage often precedes the appearance of psoriatic lesions. This phenomenon was named after him. In 1885, another Heinrich, Heinrich Auschpitz, described pinpoint bleeding when the surface of a psoriatic plaque peels off [4].
Figure 3. Early psoriasis researchers. a - Robert Willan (1757 - 1812), an English doctor who made a classic description of psoriasis in the 19th century. He belongs to the first classification of skin diseases. b - Ferdinand von Hebra (1816 - 1870), Austrian doctor, founder of modern scientific dermatology, awarded a knighthood.
website zeno.org and Wikipedia
Preventive measures
Prevention of the disease requires compliance with simple rules. Firstly, you need to protect your nervous system, because stress factors can trigger psoriasis. Secondly, it is necessary to strengthen the immune system and lead a healthy lifestyle:
- exclude fried, salty, fatty foods from the diet and eat healthy;
- do not smoke or drink alcohol, as this may worsen symptoms;
- take care of your skin - avoid frostbite, prolonged exposure to the scorching sun, avoid mechanical damage;
- wear underwear made from natural fabrics.
Literature
- Dermatovenerology. National leadership / ed. Skripkina Yu.K., Butova Yu.S., Ivanova O.L. M.: GEOTAR-Media, 2014. - 1024 pp.;
- Ruiz-Romeu E., Ferran M., Sagristà M., Gómez J., Giménez-Arnau A., Herszenyi K. et al. (2016). Streptococcus pyogenes-induced cutaneous lymphocyte antigen-positive T cell-dependent epidermal cell activation triggers TH17 responses in patients with guttate psoriasis. J. Allergy Clin. Immunol. 138, 491–499;
- Weigle N. and McBane S. (2013). Psoriasis. Am. Fam. Physician. 87, 626–633;
- Advances in psoriasis: A multisystemic guide / ed. by Weinberg JM, Lebwohl M. London: Springer-Verlag, 2014. - 340 p.;
- Baker B. S., Swain A. F., Fry L., Valdimarsson H. (1984). Epidermal T lymphocytes and HLA-DR expression in psoriasis. Br. J. Dermatol. 110, 555–564;
- Bhalerao J. and Bowcock M. (1998). The genetics of psoriasis: a complex disorder of the skin and immune system. Hum. Mol. Genet. 7, 1537–1545;
- Elder JT, Bruce AT, Gudjonsson JE, Johnston A, Stuart PE, Tejasvi T, et al. (2010). Molecular dissection of psoriasis: integrating genetics and biology. J. Invest. Dermatol. 130, 1213–1226;
- Chen M., Wang Y., Yao X., Li C., Jiang M., Cui P., Wang B. (2016). Hypermethylation of HLA-C may be an epigenetic marker in psoriasis. J. Dermatol. Sci. 83, 10–16;
- Gaskoin G. On the psoriasis or lepra. J. & A. Churchill, 1875. - 259 p.;
- Fitzpatrick D.E. and Elling D.L. Secrets of dermatology. M.: BINOM, 1999. - 512 pp.;
- van de Kerkhof PCM Textbook of psoriasis (2nd Edition). Wiley-Blackwell, 2003. - 360 p.;
- Bergstrom K.G. and Kimball A.B. Psoriasis. M.: Praktika, 2007. - 162 pp.;
- Debbaneh M., Millsop J. W., Bhatia B. K., Koo J., Liao W. (2014). Diet and psoriasis, part I: Impact of weight loss interventions. J. Am. Acad. Dermatol. 71, 133–140.