Cystitis is a common inflammatory disease of the bladder among the adult population, especially in women. Acute cystitis can become chronic with periodic exacerbations. The reasons for frequent exacerbations of cystitis in women are a short, wide urethra (urethra) and proximity to natural sources of infection - the vagina and anus. Hormonal disorders in women often lead to vaginal dysbiosis and the growth of pathogenic bacteria, which provoke frequent exacerbations of bladder inflammation. In men, symptoms of cystitis are usually associated with prostate disease.
Main symptoms of cystitis
- frequent painful urination
- pain in the groin area
- false urge to urinate
- cloudy urine, possibly containing blood
- sudden onset of symptoms
- increase in body temperature
What urine test is needed for cystitis?
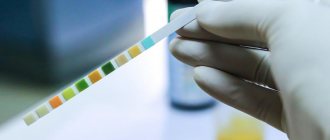
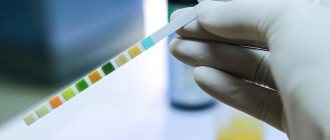
If cystitis is suspected, you must first undergo a general urinalysis (UCA). The results of OAM in cystitis will reveal an increased content of leukocytes, bacteria, and an increased content of erythrocytes and protein may occur.
Additionally, the attending physician may recommend conducting bacterial culture of urine to determine antibiotic sensitivity to identified pathogenic microorganisms, PCR diagnostics for sexually transmitted diseases, and a number of studies for the diagnosis of viral infections (since cystitis is not always caused by bacteria).
From instrumental studies, the doctor can refer the patient to an ultrasound of the kidneys, CT/MRI of the pelvis to exclude tumors and stones in the urinary system, kidney and prostate diseases in men.
Prevention of exacerbations of cystitis
- Regularly perform thorough toileting of the external genitalia
- Use barrier methods of contraception
- Timely treatment of gynecological and urological diseases
- Urinate immediately after intercourse
Symptoms and signs of infection
Depending on the type of bacterium that led to the development of escherichiosis, infection can be recognized by the following characteristic signs:
- Enteroinvasive rod. This pathogen can cause acute intoxication in both adults and children. Clinical symptoms of infection with enteroinvasive bacillus are similar to those of dysentery. Infection is indicated by frequent urges to have bowel movements (up to 25 times a day), general weakness, nausea, and stools acquire a watery consistency and may contain mucus impurities.
- Hemolytic (enterohemorrhagic, hemolyzing) bacillus. This pathogenic microorganism causes hemolytic-uremic syndrome in adults, and in children it provokes hemorrhagic colitis. Both diseases require timely treatment.
- Enterotoxigenic. Symptoms of infection with this microorganism include nausea and frequent episodes of vomiting, severe diarrhea, and cramping pain in the umbilical region. This type of intestinal infection is equally common among adults and children.
- Enteropathogenic escherichiosis. If E. coli is detected in an infant, then in 80% of cases we are talking about enteropathogenic escherichiosis. Infection can be recognized by symptoms such as diarrhea and vomiting. A newborn baby refuses to eat, there is frequent regurgitation, restlessness, continuous crying and insomnia.
Standard treatment for E. coli includes taking medications that have a detrimental effect on the microorganism, as well as drugs to eliminate the symptoms of intoxication.
Preparing for the OAM test for cystitis
On the day before taking biomaterial, it is advisable to refrain from physical activity, drinking alcohol, and not eat vegetables and fruits (beets, carrots, citrus fruits, watermelons), red wine, and multivitamins, which can change the color of urine.
Avoid taking diuretics for 48 hours before urine collection (in consultation with your doctor).
Urine should be collected before starting antibiotic therapy.
Carry out a thorough toileting of the external genitalia under the shower with soap (it is prohibited to use hygiene products with antiseptics). For men, pull back the foreskin of the penis, wash the head well with warm water, and dry with a paper towel.
Women during menstruation should place a tampon in the vagina before collecting urine and inform the attending physician that the test was performed during menstruation.
Treatment
To treat symptoms of E. coli in adults and children, the following groups of drugs are used:
- Antibacterial agents. Traditional treatment of E. coli in the urine, in the vagina in women and in the lumen of the large intestine includes taking antibiotics from the group of cephalosporins. The course of treatment is from 5 to 10 days.
- Antispasmodics and painkillers. Painkillers for the treatment of E. coli symptoms in adults and children are prescribed for severe pain. For therapeutic purposes, drugs such as Nurofen, Spasmalin, No-shpa are prescribed.
- Probiotics. This group of drugs helps restore the balance of normal microflora in the lumen of the large intestine and vagina in women.
In order for probiotics containing bifidum and lactobacilli to effectively restore microflora, their intake must be combined with prebiotics, which create a favorable environment for the proliferation of beneficial bacteria. The combination drug Stimbifide Plus, which is a metaprebiotic and contains a unique combination of fructopolysaccharides and fructooligosaccharides, has proven its high effectiveness against escherichiosis.
Metaprebiotic Stimbifid Plus provides the microflora of the large intestine and vagina with unique nutrition, thereby stimulating its reproduction. Based on the results of clinical studies, a comparative characteristic of the effectiveness of Stimbifid Plus and other drugs that affect the composition of the intestinal microflora was compiled. Metaprebiotic has proven its absolute leadership. The dietary supplement Stimbifid Plus is equally effective for the prevention of both escherichiosis and other diseases.
How to properly collect a urine test for cystitis
The average portion of urine during the first morning urination is collected in a sterile container (the first and last portions are flushed into the toilet).
Urine collection is possible at any time during the day with prior agreement with the attending physician.
When collecting urine, it is advisable not to touch the container to your body.
Before urinating, women need to spread their labia with their fingers so that foreign impurities do not get into the urine from the skin of the external genitalia.
The volume of urine for testing should be ¾ of the volume of the container. The minimum volume of urine for testing is 30 ml.
It is advisable to deliver the container with urine to the medical office within 2 hours after collecting the biomaterial.
Complications and causes of recurrence of cystitis
Untreated or undertreated acute cystitis threatens chronic cystitis, interstitial cystitis or pyelonephritis.
We have already talked about chronic cystitis.
Interstitial cystitis is considered to be cystitis without obvious direct causes causing it, but with very painful symptoms.
For its treatment, analgesics, antidepressants, antihistamines, anti-inflammatory and anticholinergic drugs and antispasmodics are used.
Acute pyelonephritis is characterized by fever, severe weakness, chills, headaches, increased sweating, nausea and vomiting.
Chronic pyelonephritis, in the inactive period, is characterized by periodic dull lumbar pain, aching in nature.
During an exacerbation, symptoms are similar to acute pyelonephritis.
Chronic pyelonephritis causes persistent hypertension.
Pyelonephritis is treated with antibacterial drugs.
Detoxification drugs and immunomodulators are also indicated.
If there is severe fever, then you need to limit the amount of protein in your daily food intake.
Treatment of chronic pyelonephritis is carried out with the same drugs, but antibiotic therapy lasts longer.
Recurrent course of chronic cystitis is observed when:
- weak immunity:
- inadequate treatment of the inflammatory process in the bladder;
- when a secondary infection occurs.
By weakening or eliminating the influence of these factors, it is possible to avoid recurrent exacerbation of chronic cystitis.
Interpretation of a general urine test for cystitis
It must be remembered that interpretation of the results of a urine test should be carried out only by the attending physician, since the results of laboratory tests are not the only criterion for making a diagnosis and prescribing appropriate treatment. They should be considered in conjunction with medical history and the results of other possible examinations, including instrumental diagnostic methods.
At the medical office, you can get personal advice from a Doctor Q service doctor on deciphering the results of a urine test during your appointment or by phone.
Color. The normal color is yellow of varying intensity. It may change when you eat certain foods and take certain medications. Whitish, dark brown or other uncharacteristic color indicates the presence of pathology. Urine should be clear.
The smell of ammonia, rotting apples or rotten meat indicates various diseases (for example, cystitis, diabetes, purulent inflammation).
Urine reaction. Normal pH is 5-7 (slightly acidic reaction). Increased acidity is characteristic of feverish conditions, renal failure, diabetes mellitus and other pathologies. An alkaline reaction is observed in chronic infectious diseases.
Density readings are used to assess kidney function. During the day, the specific gravity of urine fluctuates.
There is normally no protein in the urine (proteinuria). Its appearance is a marker of the presence of various diseases (inflammatory infectious diseases of the urinary tract, kidney pathology and others). Protein is also detected in the urine after severe hypothermia or high physical activity.
There should normally be no glucose in the urine. Its detection in a biomaterial sample may indicate the presence of diseases (diabetes mellitus, pancreatic cancer, pancreatitis, etc.), as well as severe stress and consumption of large amounts of carbohydrates.
Bilirubin is detected in hepatitis, cirrhosis, obstructive jaundice and other pathological conditions associated with liver damage.
Urobilinogen in high concentrations indicates liver damage, hemolytic jaundice, and gastrointestinal diseases. An increased amount of ketone bodies indicates a disorder in protein, carbohydrate or lipid metabolism. Nitrites indicate a urinary tract infection.
Flat epithelium is the superficially located skin cells of the external genitalia. Detection of it in urine has no diagnostic value.
Transitional epithelium is found in the kidneys, ureters, bladder and upper urethra. Single cells can be found in urine sediment in healthy people. They are found in large quantities during intoxication, after instrumental interventions on the urinary tract, with jaundice, kidney stones and chronic cystitis.
The renal epithelium in healthy people is not found in sediment microscopy. Found in patients with nephrosis and nephritis.
Red blood cells are normally present in urine in small quantities. A small number of red blood cells can be observed after sports activities, lower back injuries, hypothermia and overheating. The appearance of a large number of red blood cells in the urine can occur in various pathologies (glomerulonephritis, nephrosis, collagenosis, heart disease, sepsis, influenza, infectious mononucleosis, rubella, tonsillitis, dysentery, etc.).
Leukocytes are present in the urine of healthy people. An increased number of leukocytes in the urine of women can occur when urine is contaminated with vaginal secretions. A high content of leukocytes in the urine occurs with pyelocystitis, pyelonephritis, fever of various origins, and genitourinary tract infections.
Cylinders are cylindrical structures that are primarily composed of protein and/or cells. They are usually found in pathologies of the urinary system (glomerulonephritis, pyelonephritis, renal tuberculosis, diabetic nephropathy, chronic kidney disease, renal amyloidosis, fever, scarlet fever, myeloma, osteomyelitis, systemic lupus erythematosus, etc.).
Mucus performs a protective function and is secreted by special cells of the genitourinary system. Normally, its content in urine is insignificant, but during inflammatory processes it can increase.
Salt crystals appear depending on the pH of urine and its other properties, and diet. May indicate mineral metabolism disorders, the presence of stones, or an increased risk of developing urolithiasis.
Bacteria indicate a bacterial urinary tract infection. But they can occur when urine is contaminated with bacteria from the skin and vaginal discharge.
Hemolyzing Escherichia coli
Such E. coli may be present in the body and not manifest itself. As soon as the conditions for its development are favorable (illness, weakened immunity), hemolyzing E. coli will manifest itself.
Children suffering from large amounts of hemolyzing E. coli are prone to diathesis . Symptoms include bloating, diarrhea, constipation, mucus or green matter in the stool. It should also be noted that with hemolyzing E. coli, the patient’s temperature does not increase.
The effect of hemolyzing Escherichia coli on the body is reminiscent of Staphylococcus aureus . Hemolyzing E. coli is especially dangerous for newborns. Since even a small amount of it can disrupt normal digestion in a child.
Intestinal infection in children, prevention
We will not spend much time describing the routes of infection. In this case, the main route of infection is certainly the entry of the pathogen directly through the mouth into the human body, or with unwashed hands, or through contaminated food and hygiene items. Children most often become infected with rotavirus infection. This happens because until the age of 3, most children are especially susceptible to rotavirus, and in hot climates, where we all try to get to in the summer, rotavirus lives everywhere, even in refrigerators. This does not mean that you cannot contract any other intestinal infection. Diarrhea, for example, can be caused by the so-called “travelers' disease”, the cause of which is no longer a virus, but a bacterium - E. coli, which lives in the specific region you are visiting and enters the body usually with water, which is all local they drink, and nothing bad happens to them for this, since they all have a strong immunity to this stick, but you and I don’t have this immunity, so we are friends with the toilet for a couple of days.
But you can still protect yourself from traveler's illness: wash your hands before eating and drink only bottled water. But protecting yourself from rotavirus is much more difficult, since it can end up anywhere, including, unfortunately, getting directly into the food on the table.
Since you and I know that rotavirus loves children most of all, a logical question arises: is there a vaccine against it? Yes, I have. The vaccine against rotavirus is called Rotatec. If you immediately after the birth of your baby begin to plan some long trips a year or two after his birth, then of course it would be better to immediately take care of vaccinating your baby against rotavirus.
Attention! to get vaccinated against rotavirus after a year, since the instructions for the drug imply a three-time vaccination regimen in the period from 2 to 8 months. The vaccine is administered orally, it is a live vaccine, and it may have contraindications, so before getting vaccinated against rotavirus, you should consult with a pediatric immunologist.
Contagiousness of cystitis
Most often, as we have already discussed, infectious cystitis occurs from E. coli.
And such opportunistic microflora is not infectious to other people.
Sexual transmission of infection is not typical for cystitis.
But having unprotected sex can lead to cystitis or its relapse.
Exacerbations of cystitis are always accompanied by severe pain in the lower third of the abdomen, which serves as an obstacle to sex.
You cannot become infected with any form of cystitis directly from a person.
But by following certain rules of conduct in sexual life, you can avoid the causes that lead to cystitis.
It is necessary to be tested for STIs twice a year.
Regular sex and normal sexual activity increase your chances of not getting cystitis more than long periods of abstinence.
Timely treatment begins with a complete cure for cystitis.
And correct and regular adherence to preventive measures will help avoid recurrent cystitis.